Perceptions and Changes in Quality of Life for Caregivers of Patients with a Traumatic Brain Injury
| ✅ Paper Type: Free Essay | ✅ Subject: Family |
| ✅ Wordcount: 3395 words | ✅ Published: 23 Sep 2019 |
Pilot Survey on the Perceptions and Changes in Quality of Life for Caregivers of Patients with a Traumatic Brain Injury
Abstract
This proposed pilot study sought to examine the perceptions and changes in quality of life for caregivers of patients with a traumatic brain injury. It explored the different views and opinions of caregivers. Many people are not educated on the stress or afflictions that caregivers endure due to patients or loved ones for whom they are caring. This study explored specific cases of burdens among caregivers due to traumatic brain injury patients, how caregivers coped with their stress, and what life changes were made because of the traumatic brain injury. A better understanding of what caregivers experience would help researchers as well as the general public become more aware of how serious traumatic brain injuries are, not just for the patient, but also for the people who care for the patients.
Keywords: caregivers, patients, traumatic brain injury, stress, burdens
When a patient has a traumatic brain injury, the primary focus of care and rehabilitation is on the patient. However, the traumatic brain injury plays a significant role on the family and/or caregiver of the patient (Wells, Dywan, & Dumas, 2005). The way in which the patient responds to the injury, treatment, or support can alter life around the patient including people and activities (Lehan, Arango-Lasprilla, Reyes, & Quijano, 2012). Researchers of this proposed pilot study used the work of other authors and data obtained from other peer-reviewed articles to compare and analyze anticipated results of this study with other findings. The purpose of this study was to observe and to measure the perceptions and quality of life changes of caregivers who care for traumatic brain injury patients. This study discusses and analyzes the impact that the traumatic brain injury has on the caregiver and their quality of life.
Marsh, Kersel, Havill, and Sleigh (2002) stated that the majority of peer-reviewed sources acknowledge the benefits that caregivers give to traumatic brain injury patients (TBI), but only a select few go into detail about the stress and burden on the caregivers’ lives due to the TBI patient. They conducted an assessment of TBI caregivers at six-months and one-year post-injury to analyze their wellbeing and burdens. Caregivers of TBI patients reported increased anxiety, changes in financial situations and relationships, less time for themselves, and increased use of medication after caring for the patient for six months. The caregivers, after some time, were able to gain practical ways to cope with the changes and find ways to best serve their patients.
In a recent study, Manskow, Friborg, Roe, Braine, Damsgard, and Anke (2017) studied the quality of life of family members who cared for TBI patients at one and two years post-injury. Manskow et al. (2017) performed a study on family members of TBI patients to assess their perceptions and quality of life changes and if certain events in their lives progressed or regressed due to the injury. This study in particular discovered that caregivers experience an immense amount of loneliness. The results showed that the satisfaction of life is worse at two years post-injury than one year post-injury (Manskow et al., 2017). This study presented a need for long-term follow-up of patients and family members.
Wells et al. (2005) discovered that loved ones providing care for a family member who has experienced a TBI typically have higher levels of satisfaction with their role. They also state that the caregiver’s coping strategies allowed their health and happiness to stay present. There were some negative effects found on caregivers such as financial hardships; therefore, family income was shown to decrease. This resulted in high level stress on the caregiver.
Nabors, Seacat, and Rosenthall (2002) conducted a study to determine whether there is a correlation between demographic qualities of the caregiver and the weight of the burden on the caregiver. They also assessed the ratio of caregiver adjustment to the severity of the injury of the patient, relationship of the caregiver to the patient, social support, and perceived burden. The study determined that there was a significant impact on the family of a TBI survivor such as: stress, depression, and anxiety. All of these factors led to the decrease of healthy family functioning. A decrease in income was inversely related to the increase of the weight of a caregivers burden. However, there was no relationship between race and the weight of the burden.
Lehan, Arango-Lasprilla, Reyes, and Quijano (2012) stated that, “family caregivers are at risk for physical and emotional problems, which can negatively influence their individual and family functioning” (p. 87). These findings signified that the burdens on caregivers also indicated a change in the quality of life of the individuals with a TBI. It also indicated that the caregivers required a vast amount of ongoing support so that they could meet all of the demands of caregivers to improve their physical health, mental health, and functioning.
Perlesz, Kinsella, and Crowe (1999) aimed to perform a review of the psychological impact that a TBI had on a caregiver. One of the main factors that were measured in this study was medication usage and counseling uptake. This study observed that there was a higher rate of stress among caregivers caring for their spouses with a TBI, rather than parents caring for a child with a TBI. One aspect that was noted was that parents struggled more with behavioral impairments than with their child’s physical disability. They stressed that the relationship of the caregiver to the TBI patient caused more or less stress to the caregiver.
There were also negative effects found on caregivers, which were mentioned by Kreutzer, Rapport, Marwitz, Harrison-Felix, Hart, Glenn, and Hammond (2009). Psychologic distress such as anxiety and depression were some negative effects they encountered with caregivers of TBI patients. These effects were found to be more prevalent in caregivers of a patient whose functioning level was significantly low.
Perrin, Stevens, Sutter, Hubbard, Diaz Sosa, Espinose Jove, and Arango-Lasprilla (2013) examined the family dynamics that relate to the mental health of the caregiver of a TBI patient. According to Perrin et al., (2013), the results of the study showed that family dynamics and caregiver mental health were affiliated, stating that caregivers with high family satisfaction and cohesion tended to decrease their burden and increase their satisfaction with life and vice versa (p. 839). Depression and burden negatively affected the happiness of the caregiver/family member. It is shown that caregiver mental health would be improved in Latino populations if techniques and programming were improved.
Petranovich, Wade, Taylor, Cassedy, Stancin, Kirkwood, and Brown (2015) examined the efficacy of improving long-term caregiver psychological functions post TBI in children and adolescents. Petranovich et al. (2015) stated that the income was a big factor in psychological distress of caregivers on TBI patients. The study followed up with web-based interventions if the family members still showed dissatisfaction. The study found the web-based interventions essential for improving the psychological factors of caregivers as well as TBI patients.
Blake (2008) conducted a study to determine whether caregiving affected the caregivers emotional and physical states. She stated that it is common for the caregivers’ physical health to decline due to their focus on the patient. She also made the observation that long-term depression is common, and that their depression could have increased the longer they care for the patient. One important focus that the article mentioned is that not all caregiving experiences are negative. Some caregivers enjoyed the benefit that they received from caring for their loved one. This study suggested that providing helpful information, social support, respite care, and training and counseling for the caregiver are essential for the caregiver’s well-being.
Turner, Fleming, Parry, Vromans, Cornwell, Gordon, Shields, and Ownsworth (2010) also studied psychologic distress on caregivers. They specifically wanted to know how these psychological factors were affected during the phase of transition from the hospital to home. The study found that the distress was less prevalent the first month after leaving the hospital. Distress levels were actually higher before the patient was discharged from the hospital. They suggested that before discharge, having support services and knowledge of coping strategies would benefit the caregivers when transitioning from hospital to home (Turner et al., 2010).
Backhaus, Ibarra, Klyce, Trexler, and Malec (2010) conducted a study to determine whether there would be improvement in psychological functioning and self-efficacy if the caregivers and the survivor of a TBI were trained in coping strategies. This study developed the idea that self-efficacy could change the survivors’ emotions and adjust the emotions after the injury takes place. Results of this study stipulate that perceived self-efficacy is an essential and flexible factor in assisting and caring for the survivors’ new way of life after suffering from a TBI.
Overall, these sources suggest that caregiving for a patient with a TBI can lead to an increase in factors such as stress, anxiety, depression, financial burden, medication intake, and physical and emotional impairments. Researchers and the general public should be aware of the problems that caregivers of TBI patients face. The information collected from these scholarly articles allow the public to become more knowledgeable of this information and can increase the chance of early intervention to prevent many of these factors from being acquired. The research articles previously mentioned support our hypothesis that the perception and quality of life will negatively change in both the caregiver and the TBI patient. More specifically, this pilot study searched to find the perceptions and changes in quality of life for the caregiver of a TBI patient.
Methods
Participants
The expected participants involved in the sample were caregivers of 20 TBI patients who were recruited through social media (e.g. Facebook, Twitter) and research flyers (Addendum A) that were distributed at the Jackson Medical Mall. A homogenous sampling technique was used to select the participants for the study. Caregiver demographics included: age, gender, level of education, employment status, years of experience, yearly income and location of services. Patient demographics included: age at occurrence of TBI, cause of TBI, and living situation.
Measures
A structured survey (Addendum B) with an average completion time of five minutes, was completed by all caregivers who participated in the study. The survey used multiple choice questions and quality of life ratings for ease of completion. The survey consisted of 20 questions beginning with 10 demographic questions. Data collected from this survey included caregivers’ demographics such as: age, gender, level of education, employment status, years of experience, yearly income, and location of services. These questions were selected by the researchers to discover if caregiver attributes affected their quality of life. Also, 10 quality of life questions were included in the second half of the survey. The results were stored in Qualtrics.com and the facilitator’s office for the use of educational purposes only. The researchers collected and interpreted data. The data was analyzed and averaged to get an overall perspective of the perception of quality of life changes in caregivers post TBI.
Procedure
The caregivers were asked to participate in a short, online survey to assess caregivers’ perceptions of their quality of life following the TBI of the patient. The survey was created using Qualtrics.com. Once the caregivers agreed to participate in the study, researchers of the study sent an email asking the participants to complete a consent form (Addendum C) and sign the form in order to maintain the integrity and privacy of data. Once participants completed and returned the consent forms to the researchers, a direct link to the survey and instructions were emailed to the caregivers. Once the participants submitted their answers on Qualtrics.com, the results were available for researchers to view and analyze.
Data analysis
A descriptive statistical analysis approach was used to examine the caregivers’ perceptions and changes in quality of life following a TBI.
Results
The researchers expected 20 responses to the survey presented via Qualtrics.com. There were zero completed surveys. For the missing data, measures were anticipated by the researchers based on each survey question. The measures included demographic information from the caregiver and the patient and the perception of quality of life changes in caregivers. For the purposes of discussing individual factor’s relatedness and predictor power, researchers of this study have anticipated each measure separately.
Descriptive Data
The researchers expected that the majority of aspects of quality of life would become worse for the caregiver after the patient’s TBI. The caregivers responded that their marriage/romantic relationships, interpersonal/social relationships, employment, income, general health, parenting, and psychological status became worse after the patient’s TBI. Aspects that were expected to have no change for the caregiver included the caregiver’s education and their living situation. These results are exhibited in Figure 1. As for the TBI patient, the caregiver’s expected responses included deterioration of the patient’s relationship with family and friends, marriage/romantic relationships, education, employment, income, and/or living situation. These results are exhibited in Figure 2. 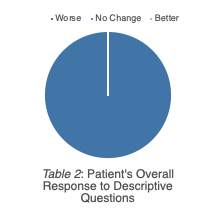
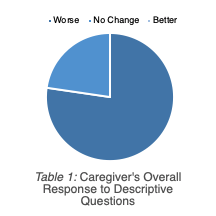
Most of the caregivers reported that the patient that they were caring for did not have a disability prior to their injury. In most cases, the researchers expected that the survivor was admitted to the hospital post-TBI due to substantial injuries. Most patients were expected to receive home health services and outpatient therapy. Many patients were currently receiving speech therapy, occupational therapy, physical therapy, and psychological counseling. A majority of the participating caregivers belonged to a caregiver support group prior to the survey. The caregivers asserted a suitable living arrangement was provided for their patients’ needs. Frequent responses included caregivers who provide moderate assistance to the patients with a TBI.
Demographic Variables
Since data was not obtained from the survey, the results were anticipated by the researchers. The researchers discovered that the majority of the predicted responses came from caregivers who were adults (between the ages of 21-64). Results showed that the patients that caregivers were caring for were also adults (between the ages of 21-64). The majority of predicted responses came from female caregivers; therefore, there was not enough information or data on male caregivers to assess the impact of gender. Most caregivers had a Bachelor’s degree level of education. Responding caregivers reported having more than five years’ experience with caring for a TBI patient. The majority of expected responses outline that caregivers surveyed cared for the patient at home. Most patients lived at home but needed assistance from a caregiver for functional everyday activities. The expected participants reported being employed part-time with an average income between $20,000 and $40,000 per year. The researchers would expect that the cause(s) of the TBI would vary considering the many possible causes of a TBI, such as motorcycle/motor vehicle accident, gunshot wound, or sports injury.
Discussion
The purpose of this survey was to assess the relationship of perceptions of quality of life changes in caregivers of TBI patients. The anticipated results indicated a pattern of increased burden on caregivers related to the survivors’ injury and the caregivers’ perceptions of the survivors’ difficulties and dysfunctions. Caregivers’ anticipated burden remained relatively constant throughout the years post injury as reported by Marsh et. al (2002). The caregivers’ environmental context regressed but remained constant post-injury. Our anticipated results show that the caregivers’ quality of life regressed, but after a few years, there were no more changes. The studies previously mentioned (Backhaus et al., 2002; Blake, 2008; Kreutzer et al., 2009; Lehan et al., 2012; Manskow et al., 2017; Marsh et al., 2002; Nabors et al., 2002; Perlesz et al., 1999; Perrin et al., 2013; Petranovich et al., 2015; Turner et al., 2010; and Wells et al., 2005) support and are consistent with our findings.
Several similarities were found regarding the researcher’s literature review on similar peer-reviewed articles and this study. Marsh et al. (2002) reported increased anxiety, increased use of medication, and negative changes in financial situations and relationships. Nabors et al. (2002) stated that stress, anxiety, and depression led to the decrease of healthy family functioning. Lehan et al. (2012) reported that caregivers require a vast amount of ongoing support to meet demands of physical and mental health as well as their functioning. Perlesz et al. (2014) stated that depending on the relationship of the caregiver to the TBI patient caused more or less stress to the caregiver. They also stated that there was a higher rate of stress among caregivers caring for a spouse, rather than a caregiver caring for a child. Perrin et al. (2013) reported that caregivers with high family satisfaction and cohesion tend to have a low burden and a high satisfaction with life. Blake (2008) suggested that providing helpful information, social support, respite care, training, and counseling for the caregiver are essential for the caregiver’s well-being. The findings of the pilot study showed that the caregiver of the TBI patient perceptions and quality of life decreased in most aspects. The perception and quality of life of the TBI patient decreased as well.
Clinical implications may include treatment for caregivers in psychological, cognitive, physical, occupational, and communicative aspects. Support groups lead by professionals such as psychiatrists, psychologists, speech-language pathologists, and other counselors may positively impact the caregivers. These support groups may decrease caregivers’ stress by communicating with other individuals and families who have faced similar challenges.
To allow additional caregiver insight, the researchers included more detailed questions in the survey regarding, which type of psychological distress they experienced such as depression and anxiety. Anticipated limitations may result from having a majority of female caregivers that responded to the survey and few to no male caregivers. The psychological aspects in men and women vary, therefore less information about psychological stress may be addressed.
Future research should include more in-depth questions for the caregiver to determine a more specific perception of quality of life rather than a broad overview. The research would benefit from a larger, more diverse sample to decrease the chance of response bias. This would increase reliability and validity of the research being conducted.
References
- Backhaus, S. L., Ibarra, S. L., Klyce, D., Trexler, L. E., & Malec, J. F. (2010, June). Brain injury coping skills group: A preventative intervention for patients with brain injury and their caregivers. American Congress of Rehabilitation Medicine, 91, 840-848. doi: 10.1016/j.apmr.2010.03.015
- Blake, H. (2008, April 21). Caregiver stress in traumatic brain injury. International Journal of Therapy and Rehabilitation, 15(6), 1-29.
- Kreutzer, J. S., Rapport, L. J., Marwitz, J. H., Harrison-Felix, C., Hart, T., Glenn, M., & Hammond, F. (2009, June). Caregiver’s Well-Being After Traumatic Brain Injury: A Multicenter Prospective Investigation. American Congress of Rehabilitation Medicine, 90, 939-946. doi:10.1016/j.apmr.2009.01.010
- Lehan, T., Arango-Lasprilla, J. C., de los Reyes, C. J., & Quinjano, M. C. (2012, January). The ties that bind the relationship between caregiver burden and the neuropsychological functioning of TBI survivors. NeuroRehabilitation, 30(1), 87-95. doi:10.3233/NRE-2011-0730
- Manskow, U. S., Friborg, O., Roe, C., Braine, M., Damsgard, E., & Anke, A. (2017, August 18). Patterns of change and stability in caregiver burden and life satisfaction from 1 to 2 years after severe traumatic brain injury: A Norwegian longitudinal study. NeuroRehabilitation, 40(2), 211-222. doi:10.3233/NRE-161406
- Marsh, N. V., Kersel, D. A., Havill, J. H., & Sleigh, J. W. (2002). Caregiver burden during the year following severe traumatic brain injury. Journal of Clinical and Experimental Neuropsychology, 24(4), 434-447. doi: 10.1076/jcen.24.4.434.1030
- Nabors, N., Seacat, J., & Rosenthall, M. (2002, April 22). Predictors of caregiver burden following traumatic brain injury. Brain Injury, 16(12), 1039-1050. doi:10.1080/02699050210155285
- Perlesz, A., Kinsella, G., & Crowe, S. (1999). Impact of traumatic brain injury on the family: A critical review. Rehabilitation Psychology, 44(1), 6-35. doi:10.1037/0090-5550.44.1.6
- Perrin, P. B., Stevens, L. F., Sutter, M., Hubbard, R., Diaz Sosa, D., Espinose Jove, I. G., & Arango-Lasprilla, J. (2013, October). Exploring the connections between traumatic brain injury caregiver mental health and family dynamics in Mexico City, Mexico. American Academy of Physical Medicine and Rehabilitation, 5(10), 839-849. doi: 10.1016/j.pmrj.2013.05.018
- Petranovich, C. L., Wade, S. L., Taylor, H. G., Cassedy, A., Stancin, T., Kirkwood, M. W., & Brown, T. M. (2015, August). Long-term caregiver mental health outcomes following a predominately online intervention for adolescents with complicated mild to severe traumatic brain injury. Journal of Pediatric Psychology, 40(7), 680-688. doi:10.1093/jpepsy/jsv001
- Turner, B., Fleming, J., Parry, J., Vromans, M., Cornwell, P., Shields, C., & Ownsworth, T. (2010, December). Caregivers of adults with traumatic brain injury: The emotional impact of transition from hospital to home. Journal of the Australasian Society for the Study of Brain Impairment, 11(03), 281-292. doi:10.1375/brim.11.3.281
- Wells, R., Dywan, J., & Dumas, J. (2005, December). Life satisfaction and distress in family caregivers as related to specific behavioural changes after traumatic brain injury. Brain Injury, 19(13), 1105-1115. doi:10.1080/02699050500150062
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allDMCA / Removal Request
If you are the original writer of this essay and no longer wish to have your work published on UKEssays.com then please click the following link to email our support team:
Request essay removal


