Total Cost of Illness Analysis
| ✅ Paper Type: Free Essay | ✅ Subject: Economics |
| ✅ Wordcount: 1552 words | ✅ Published: 13 Oct 2017 |
1. Introduction:
By analyzing recent health related data and health activities it seems that positive changes has been initiated in Bangladesh health care system. Some health indices progress praised by internationally such as maternal and infant mortality, vaccination, birth control, cholera and arsenic prevention. Government as well as private sector spread the services to the rural area. The quality of health care drastically changed in Bangladesh in the past 20 years. But expenditure of health care or total cost of illness increasing day by day. Due to rising cost of illness or financial burden poor and marginalized people suffering to get better health care services. Existing cost barriers and quality weakness deter use of health care, especially by the poor (Sauerborn, R., Adams, A. et al., 1996). According to Household Income and Expenditure Survey 2010, 15.57 percent could not get access to health care service (Non-treatment) due to high cost of treatment. Every year 100 million people face poverty and another 150 million people suffer due to catastrophic health care cost (WHO, 2010). Recent ICDDR’B study reveals that around 6.4 million or 4 percent people in Bangladesh get poorer every year due to excessive health cost (The Daily Star, 2014).
This study focused on the total cost of illness occurred at the household level from several direction. Analysis for total cost of illness is extremely important because it helps policy makers such as the World Bank, World Health Organization, and National Government to develop ways to protect household from financial (economic) burden of illness. Sometimes this type of research led to change policy- the World Bank withdraw its plea for introducing fees in health sector, which governed its policy discourse in 1980s and 1990s (Sakdapolarak, P., Seyler, T. et al. 2013). Cost of illness studies made significant contribution to quantifying and documenting the health outcome values (Rice, P. D., 2000).
In Bangladesh, in absent of inadequate health insurances public, private health care providers adopted pre-payment mechanism. Where pre-payment mechanism are activated, citizens are forced to pay out-of-pocket from their income and get access barrier to health care due to high cost (Xu, K., Evans, D. B. et al. 2007; WHO, 2010).
Illness enforced high financial burdens on patients as well as their families. Direct and indirect costs of illness were significant but indirect costs were the dominant cost component, financial burden of treatment vary depends on type of diseases (Russell, S., 2004; McIntyre, D. et al., 2006). In many countries, high financial burden occurred due to health service weakness such as poor quality of health care, low coverage, registration fee (Chuma, J. et al. 2007).
Economic or financial burden (effects) depend not only upon the direct cost of treatment but also upon the indirect cost. According to Doorslaer, E. V., O’Donnell, O., et al. (2005) expenditure for health care in developing countries laying people into poverty risk not only in rural area but also in urban areas. In Bangladesh, the richest household spend on average 9% of household budget on health care, while the poorest spend on average 3%. The poorest household spends a larger fraction of their resources on health care compared to the richest household (Doorslaer, E. V., O’Donnell, O., et al. 2005).
For literature review systematic searches were conducted using the key words illness, total cost, direct cost, indirect cost, household, financial burden. Different author used different methodologies to measure total cost of illness, used different technique to analysis and present data. So that it was challenging to measure the total cost of illness for outdoor patients because there was not much literature review for outdoor patients.
3. Study area, Data Collection and Methods:
3.1 Study Area and Data Collection
This study conducted in a divisional city Sylhet which is situated north-eastern of Bangladesh. Ten enumerators (university student) were trained to collect data. Data were obtained in 2011via face to face interview from 252 outdoor patients from one public medical college MAG Osmani Medical College Hospital and two private medical college hospitals viz. Jalalabad Ragib Rabeya Medical College & Hospital, Women’s Medical College & Hospital and compared the total cost of illness. In every hospital, each patients got a serial number when they paid the registration fee. Everyday those number collected from hospital administration and patients were randomly chosen. For data collection process strictly followed the random sampling process to avoid selection bias. To collect the data from the patients, enumerators waited in front of doctor’s office for the patients assigned with a randomly selected serial number. After consultation when the patients exited from the doctor’s office enumerators provided the some basic information about the research study to get their cooperation in data collection. This study followed Abdur Razzaque Sarker et al.’s (2013) for sampling design.
Note that outdoor patient of public hospital MAG Osmani Medical College hospital charged a nominal registration fee. This public hospital provided common medicine free within the registration fee to the outdoor patient and also provided common diagnostic services with cheaper price. While private hospitals charged a higher registration fee compared to public hospital but did not provide any medication free.
3.2 Methods
To measure the total cost of illness this study used the incidence-based approach. A structured questionnaire was designed to collect data including all components of direct cost medical cost, direct non-medical cost, indirect cost, illness details and socio-economic status. Direct medical costs included hospital’s registration fee, medicine cost, diagnostic cost and direct non-medical costs included transport cost, informal payments. Analysis were done using SPSS V 20 for windows and data were presented as a total and as an average costs in both US dollar and Bangladeshi Taka (local currency).
Indirect costs were the income loss or social productivity loss and using the human capital approach indirect costs were measured. For simplicity:
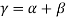
Where  was indirect cost,
was indirect cost,  was income loss and
was income loss and  was social productivity loss. Income loss defined by the loss of income during the illness. Social productivity loss occurred when patients (and parents/ family member in case of child) could not work due to illness. Social productivity loss measured by:
was social productivity loss. Income loss defined by the loss of income during the illness. Social productivity loss occurred when patients (and parents/ family member in case of child) could not work due to illness. Social productivity loss measured by:
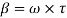
Where  was the per day income and
was the per day income and  was the number of days suffered for illness.
was the number of days suffered for illness.
Outliers were identified using the Interquartile Range (IQR). According to Tukey, J. W. (1977) and Hoaglin, D.C. et al. (1986) Interquartile Range followed the following method:

Where,  and
and  are the lower and upper quartiles respectively and g = 1.5.
are the lower and upper quartiles respectively and g = 1.5.
Tukey, J.W. (1977) proposed the outlier labeling methodology and Hoaglin, D.C. et al. (1986) stated the outlier labeling rule based on research, found that the value of g is 1.5 as a multiplier. Then outlier’s values were replaced by the series mean of corresponding variable.
4. Results and Discussions:
5. Conclusion:
Causes to high public cost:
In public health sector, pro-poor policies such as waivers are relatively ineffective to protecting household from financial burden (McIntyre, D. et al., 1995).
Public health system cannot protect household from indirect cost of illness such as wage losses and people feel discourages to use public health system due to low quality of health care services (Russell, S. J., 2001).
It is not possible to protect household from illness cost especially from non-medical direct cost and indirect cost (Russell, S., 2004).
Need further research to find out question how household manage those cost and what is the impact of total cost of illness on household assets.
6. Reference(s)
1. Steven Russell, 2004. The economic burden of illness for household in developing countries: A review of studies on Malaria, Tuberculosis, and Human Immunodeficiency virus/ acquired immunodeficiency syndrome, American Journal of Tropical Medicine and Hygiene, 71 (2), 147-155.
2. Household Income and Expenditure Survey Report 2010, 2014. Bangladesh Bureau of Statistics, Statistics and Informatics Division, Ministry of Planning, Government of Bangladesh (GoB).
3. The Daily star, 2014. Medicare too costly 4 pc get poorer every year, Dhaka, Bangladesh. Available at: http://www.thedailystar.net/4pc-get-poorer-every-year-11986 (accessed March 6, 2014).
4. World Health Report: Health System Financing- The path to Universal Coverage, 2010. World Health Organization (WHO), Geneva, Switzerland.
5. Patrick Sakdapolrak, Thomas Seyler, Christina Ergler, 2013. Burden of direct and indirect cost of illness: Empirical findings from slum settlements in Chennai, South India, Progress in Development Studies, 13 (2), 135-151.
6. Eddy Van Doorslaer, Owen O’Donnell, et al., 2005. Paying out-of-pocket for health care in Asia: catastrophic and poverty impact, Working paper no.2, EQUITAP Project.
7. Sauerborn, R., Adams, A., Hien, M., 1996. Household strategies to cope with the economic costs of illness, Social Science & Medicine, 43 (3), 291-301.
8. Diane McIntyre, Michael Thiede, Göran Dahlgren, Margaret Whitehead, 2006. What are the economic consequences for household of illness and paying for health care in low-and middle income country contexts?, Social Science & Medicine, 62 (4), 858-865.
9. Jane Chuma, Lucy Gilson, Catherine Molyneux, 2007. Treatment-seeking behaviour, cost burdens and coping strategies among rural and urban household in Coastal Kenya: an equity analysis, Tropical Medicine and International Health, 12 (5), 673-686.
10. Di McIntyre, Gerald Bloom, Jane Doherty, Prem Brijlal, 1995. Health expenditure and finance in South Africa, Health System Trust, Durban.
11. Abdur Razzaque Sarker, Ziaul Islam, et al., 2013. Cost of illness for cholera in a high risk urban area in Bangladesh: an analysis from household perspective, BMC Infectious Diseases, 13: 518.
12. Steven John Russell, 2001. Can households afford to be ill?: the role of the health system, material resources and social networks in Sri Lanka, PhD thesis, London School of Hygiene & Tropical Medicine.
13. Dorothy P. Rice, 2000. Cost of illness studies: what is good about them?, Injury prevention, 6, 177-179.
14. Tukey, J. W., 1977. Exploratory Data Analysis Reading, MA: Addison-Wesley.
15. Hoaglin, D.C., Iglewicz, B., Tukey, J.W., 1986. Performance of some resistant rules for outlier labeling, Journal of American Statistical Association, 81 (396), 991-999.
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allDMCA / Removal Request
If you are the original writer of this essay and no longer wish to have your work published on UKEssays.com then please click the following link to email our support team:
Request essay removal


