Reproductive Systems in Males and Females
| ✅ Paper Type: Free Essay | ✅ Subject: Biology |
| ✅ Wordcount: 2754 words | ✅ Published: 06 Jun 2018 |
NAME : BENJAMIN NHANDARA
Human Reproduction, Growth and Development
All living organisms reproduce and it is one of their main characteristics. Living organisms can produce a new member of species replacing those who might die due to old age, competition or in some cases being attacked by diseases. The process is known as reproduction (Clamp, A. 2005). Sexual reproduction involves two beings, male and female who have sex organs which produce gametes (sex cells) which then fuse together to form a new being. (M. B. V. Roberts, 2000).
The journey begins in the male reproductive system. Hanging outside the pelvic cavity of a man lies a sack of skin which is known as a scrotum. Present in the scrotum are muscles which move the testicles slightly depending on the surrounding temperature. The scrotum contains the male reproductive organs testes that come in pairs. In the scrotum are muscles known as cremasteric muscles. Australia, H (2016) states that the scrotum helps to maintain the temperature of the sperm at slightly below body temperature (important for sperm manufacture).
The testes are the male primary sex organs which are oval and made of fibrous connective tissue. Producing male gametes (spermatozoa/sperm) is their main function. Each testis consists of approximately 300 lobules which are separated by connective tissue and filled with seminiferous tubules, were sperm cells are produced by meiosis as stated by McGuinness, H (2010). They are tightly coiled tubules. Interstitial cells also known as Leydig cells are found adjacent to the seminiferous tubules in the testicles. They promote the secretion of male sex hormone, testosterone.
Production of male gametes begins at puberty (when a boy begins to develop into an adult, usually average age is 12 years in a male. Sperm contains the X and Y chromosomes (genetic information encoded with genes). The epididymis lies along the border of each testis and are long coiled tubes leading from the seminiferous tubules to the vas deferens. They store immature sperms until ready to be released by ejaculation (Centre, N.H.F. 2011). Long tubes known as vas deferens (sperm duct) are made of blood vessels and connect to the urethra. Sperm is released to the ejaculatory duct through the vas deferens. Short tubes join to the urethra from the seminal vesicles and semen passes through these tubes during ejaculation. The tubes are ejaculatory ducts and pass through the prostate gland. A muscular structure known as the urethra keeps urine in the bladder until excretion can occur. It provides a pathway for the flow of urine and secretion of semen. A sphincter muscle is there to prevent both functions occurring at the same time (McGuinness, H 2010).
Penis is the main external male sex organ, surrounded by erectile and connective tissue. A foreskin (folded skin) covers the tip of the penis and has many sensory receptors. The penis hangs out the pelvic cavity and excretes urine a waste product. This main organ also penetrates and ejaculates semen inside the female reproductive organ during sexual intercourse (Chard, 2001).
Males have reproductive accessory sex glands which are the Cowper’s glands also known as bulbourethral gland, prostate gland and the seminal vesicle. Chard (2001), goes on to say that the Cowper’s gland secretes a fluid that contributes to the seminal fluid, the secretion is less than that of the prostate gland. A pair of glands make the Cowper`s glands and they open into the urethra at the base of the penis. The prostate gland is like the size of a walnut and it is found in the pelvic cavity in front of the rectum and behind the symphysis pubis. A thin, milky fluid is secreted during ejaculation to enhance the mobility of sperms. Then again thick mucus-like fluid which forms 60% of semen is secreted by the seminal vesicle (M. B. V. Roberts, 2000). The fluid is alkaline and contains nutrients that are added to sperm cells. Located above the urinary bladder, highly coiled tubular structures are the seminal vesicles.
MALE REPRODUCTIVE SYSTEM
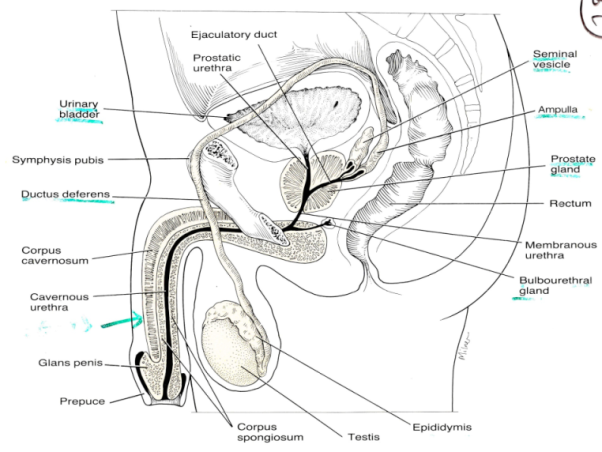
Figure 1 (eMedicineHealth,2017)
The female reproductive system is adapted so that an egg cell (gamete) can be produced and then fertilized by a sperm cell. The developing offspring is carried by the female being provided with nutrition until it is ready to be born. After birth nourishments are provided to the new infant by the female. This is all made possible by the way the female reproductive system is structured and functions.
Ovaries are female reproductive parts that come in pairs one on either side of the uterus. They produce gametes (eggs) by a process known as ovulation. Hormones oestrogen and progesterone are also secreted by ovaries. Eggs are produced by a structure called the cortex and held in a vessel inside the medulla. The ovaries attach to the uterus by ligaments known as ovarian ligaments. About 2 million immature eggs are contained in the ovaries (Chard 2001).
The fallopian tubes are muscular and lined with ciliated cells. They are about 5cm long, extend from the sides of the uterus. Other names like the oviduct or uterine tubes is used for the fallopian tube. At the end of each fallopian tube are finger-like projections known as fimbrae which receive the released eggs and transfer them to the uterus. Fertilisation also takes place in these tubes. In front of the rectum is a vast area known as the uterus. The uterus is a pear- shaped muscular chamber that has thick walls (McGuinness, H 2010). The cervix is the neck of the uterus and it opens into 2 upper corners. The uterus wall is composed of three layers of tissue, the perimetrium which is the outer layer which covers the top part of the uterus. The middle layer is known as the myometrium (middle layer of smooth muscle fibres). It is responsible for the contractions during period of labour. Finally, the third layer is the endometrium (soft with thick layer of compound tubular glands). This area is shed off each month during menstruation (Care of the mother and baby during labour, 1977).
An 8-10cm muscular and elastic tube called the vagina connects the internal female reproductive organs with the external. It discharges fluids like menstrual fluid, urine and mucus. Male semen is received by the vagina and it also provides a passage way for childbirth. Outer wall stretches during sexual intercourse.
The external genital organs of the female are collectively known as the vulva. They consist of the labia majora (thick folds of skin where pubic hair grows), labia minora (which are lip-like flesh at the entrance of the vagina), clitoris (contains erectile tissue and suspensory ligament that connect to the symphysis pubis), opening of the urethra and opening of the vagina. The main functions of the vulva are urination, menstruation, childbirth and sexual behaviour.
THE FEMALE REPRODUCTIVE SYSTEM

Figure 2 (Human Body Diagram, 2016)
A female goes through a 28-day cycle known as the menstrual or the ovarian cycle. The female menstrual cycle is divided into 4 phases. The first phase is known as proliferative phase which occurs on day 2 of the cycle. The hypothalamus releases a hormone known as Gonadotropin- releasing hormone(GnRH). The GnRH hormone is responsible for the secretion of luteinising hormone (LH) and follicle-stimulating hormone (FSH) from the pituitary gland.
The FSH secreted by the pituitary gland will stimulate the development of several ovarian follicles. A hormone called oestrogen is then secreted by the follicle on day 6 because of the chemical messenger FSH and the follicle develops into graafian follicle. Oestrogen inhibits the secretion of FSH by the pituitary gland on day 14. The layer lost in the previous menstruation is replaced by the proliferation of the endometrium. All repairs will be complete by day 14. The same hormone oestrogen will cause the secretion of LH hormone by the pituitary gland. The rapid increase in LH hormone will trigger the release of the mature egg from the ovary to the fallopian tube around day 14. This phase is referred to as the ovulation phase
In the next stage, there is secretion of nutrients by the endometrium in preparation for the implantation and this stage is the secretory phase. An endocrine structure known as the corpus luteum secretes oestrogen and progesterone. The progesterone inhibits the production of FSH. No new follicles are stimulated, the endometrium is maintained by the high levels of progesterone. A rupture of the uterine capillaries will occur when a decrease in oestrogen and progesterone levels occur. Endometrium is lost from the body as a waste product through the cervix, together with some blood. This process is known as menstruation. Hormonal changes will prepare the uterus for pregnancy but in the event, that the egg is not fertilised then the lining of the uterus is lost through the vagina (menstrual period). Figure 3 clearly shows the 28-day cycle and the different periods that a female goes through during her menstrual cycle.
FEMALE MENSTRUAL CYCLE
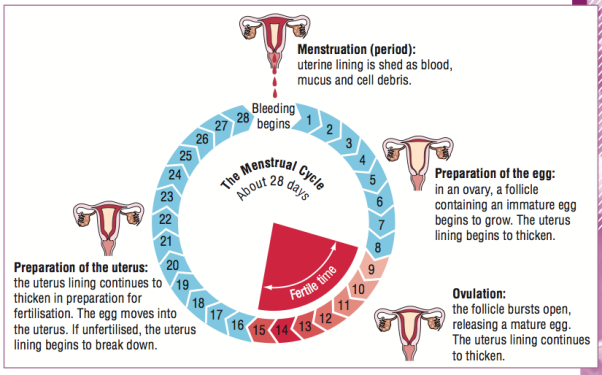
Figure 3 (Menstrupedia.com, 2017)
FEEDBACK MECHANISM INVOLVED IN THE MENSTRUAL CYCLE
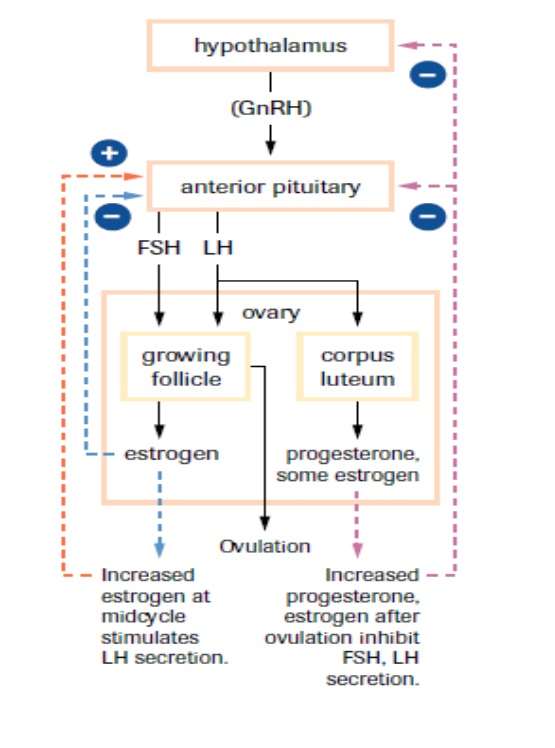
Figure 4 (SBI4U 2013 Resource Guide, 2017)
In figure 4 the effects of positive and negative feedback mechanisms are evidenced through the different responses given to different conditions at different periods of progress in the female cycle.
The result is different if the egg gets fertilised. When the mature female egg in the fallopian tube fuse with a male gamete cell due to having had sexual intercourse. The fusion of the male and female gametes to form a zygote is known as fertilisation (Clamp, A. 2005).
During sexual intercourse millions of sperms are deposited into the female reproductive tract. Sperms are smaller than the female gametes and because of their structure (having a head containing the haploid nucleus), a tail (flagellum) for mobility. The sperms swim towards the mature egg through the cervix during ovulation (Bennet, 1985). Only a few hundred sperms get close to the egg because many will die of the acidic environment and some will flow out of the vagina.
Early in pregnancy the embryo secretes hCG (human chorionic gonadotrophins). This hormone enables the corpus luteum to continue to produce progesterone, thereby preparing the lining of the uterus for the developing embryo. By testing for HCG in urine, it is easy to diagnose for pregnancy very early. Another hormone is the human chorionic somatomammotropin (HCS) also referred to as human placental lactogen (hPL). The hormone is secreted from the placenta to modify the metabolic state of the mother during pregnancy (mother`s glucose usage and release of fatty acids).
Gray, (2012) says that childbirth is divided into three stages. The woman`s age, size of uterus and the number of previous pregnancies will determine the duration of the stages. Dilation is the first stage, were the cervix dilates because the foetus would have begun its descent a few days or weeks earlier. Uterus muscle wall contract rhythmically and the head of the baby breaks the amnion and the fluid is released. Dilation of the cervix can last to 6 – 12 hours.
As the contractions of the uterus become strong, the baby is then forced out through the cervix down the vagina. This is called the delivery stage and can be 1 -2 hours. Oxytocin hormone stimulates powerful contractions that help to open the cervix to push the baby and placenta out and limit bleeding at the site of the placenta. While the “fight or flight” hormone (adrenaline) can slow the labour for the fearful females. It can be produced in large quantities because of fear (Bennet, 1985).
The umbilical code is tied and cut once the baby has begun to breathe or cry (can live independently without the placenta). After birth is the last stage which starts immediately after child birth and ends with the placenta expulsion. There is the production and ejection of milk from mammary glands (Institute4learning.com, 2017). The process is known as lactation. Prolactin hormone (mothering hormone) helps to prepare a woman for breastfeeding. Eventually the uterus will grow smaller because of the continued contraction. While nursing, 5 – 10% of women become pregnant again.
To fully go through the human life, they are stages that need to be accomplished. They are about 12 different stages and we will look at infancy or the developing child in detail. During child infancy (0-3 years), a child will become more independent as they grow and the body matures. The baby learns how to walk, talk, feed themselves. A lot of the children do not get to walk in the first year as their bones will be weak to support the weight. By being encouraged the child will experiment and develop more confidence in the ability to co-ordinate themselves (Institute4learning.com, 2017). Motor movement is the title given to the development of co-ordination movement. As early as 3 months the baby will develop different sounds. Sounds are used to show pleasure, laugh or cry as a way communicating their needs. At this stage the child will like to play so much.
Many hormones are involved in the development of the child at this stage. The most important hormone that is present is the human growth hormone (hGH) which influences the growth of bone and muscle tissue. Sometimes the overproduction of this hormone will cause the child to grow too fast and too much, while the opposite (underproduction) will cause dwarfism (Richards, M 1990).
In the journal by Richard, M. (1990) insulin is another important hormone that is found at this stage and is secreted by the pancreas. Insulin helps in the regulation of glucose levels in the blood and thereby indirectly positively contributes to growth and development. This hormone should work in collaboration with other hormones to ensure normal growth. For normal growth, the child will need sufficient energy coming from metabolic reactions (rate of reactions). These are influenced by the amount of a hormone known as thyroxine being produced by the thyroid gland. Cretinism is a condition that will develop when there is under development of thyroxine. Poor mental, physical and even retardation can be caused by underproduction.
At this stage the child likes to play. Playing helps the child to develop emotionally, physically, mentally and social development. The child should be encouraged to be active. Environmental factors such as housing and someone to play with or read to them can affect the development of the child (Lohoar, S et al. 2014)
. When a child plays with toys it helps to strengthen their muscles and improve co-ordination (physical development). The child should grow healthy by having nutritious food and hygienic. The immune system needs to develop which will safeguard the child from virus or bacterial attacks. These factors are biological factors (Chard, 2001).
Without the presents of interpersonal relationships, the child may be affected in their social development. The relationships help the child appreciate and respect of authority. It helps them to build social skills such as communication, friendship and understanding the roles of others around them. Generally, they just three factors that may affect the development of the child`s growth. The factors are biological, environmental and social or emotional as explained above (Ford, n.d.).
REFERENCES
Bennet, P. (1985). Dhaagicw Life-Stages: A Study in Paradigmatic Reconstruction. History in Africa, [online] 12, pp. 11-28. Available at: http://dx.doi.org/10.2307/3171709 [Accessed 24 Mar. 2017].
CARE OF THE MOTHER AND BABY DURING LABOUR. (1977). InPharma, [online] 110(1), pp. 11-11. Available at: http://dx.doi.org/10.1007/bf03289422 [Accessed 18 Mar. 2017].
Centre, N.H.F. (2011) The male reproductive system. Available at: http://www.fertilityhandbook.com/pages/reproductive-health-overview/male- reproductive-system.php (Accessed: 20 March 2017).
Chard, T. (2001). Does the baby gain weight during labour? Human Reproduction, [online] 16(2), pp.207 [Accessed 22 Mar. 2017]
Clamp, A. (2005) As/a-level biology essential word dictionary (essential word dictionaries). United Kingdom: Philip Allan Updates.
EMedicineHealth. (2017). The Male Anatomy: Pictures, Diagrams & Reference. [online] Available at: http://www.emedicinehealth.com/script/main/mobileart- emh.ssp?articlekey=59149 [Accessed 22 Mar. 2017].
Ford, J. (n.d.) Growth & development.
Human Body Diagram. (2016). Human Body Diagram – Anatomy Human Labelled And Chart. [ONLINE] Available at: http://humananatomyclas.com/wp- content/uploads/2016/10/female-reproductive-system-function-female-reproductive- system-functions-anatomy-human-body.jpg [Accessed 24 Mar. 2017].
Institute4learning.com. (2017). The 12 Stages of Life / Thomas Armstrong, Ph.D..[online] Available at: http//www.institute4learning.com/resources/articles/the-12-stages-of- life/ [Accessed 23 Mar. 2017]
Lohoar, S., Butera, N., Kennedy, E., Child Family Community Australia. And Australian Institute of Family Studies. 92014) Strengths of Australian aboriginal cultural practises in family life and child rearing. Australian Institute of Family Studies.
Menstrupedia.com. (2017). Friendly guide to healthy periods-Menstrupedia. [online] Available at: https:www.menstrupedia.com/articles/physiology/cycle-length [Accessed 22 Mar. 2017].
McGuinness, H. (2010) Anatomy and physiology: Therapy basics. 4th edn. London: Oxford University Press.
Richards, M. (1990) “Infant crying, sleeping and feeding,” JOURNAL OF Reproductive and infant Psychology, 8(4), pp. 274-277. doi: 10.1080/02646839008403644.
Roberts, M.B.V., Reiss, M.J., Monger,G. and Robert.., M.B.V. (2000) Advanced biology. United Kingdom: Nelson Thornes
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allDMCA / Removal Request
If you are the original writer of this essay and no longer wish to have your work published on UKEssays.com then please click the following link to email our support team:
Request essay removal


