Development of Care Plan for Person with Dementia
| ✅ Paper Type: Free Essay | ✅ Subject: Health And Social Care |
| ✅ Wordcount: 3198 words | ✅ Published: 23 Sep 2019 |
Specific Needs of the Older Person
Introduction
Dementia is characterized by cognitive decline or behavioral (neuropsychiatric) changes in relation to a previous level of performance that causes loss of independence for activities of daily living. Alzheimer’s disease and vascular dementia are the main forms of dementia in the elderly, accounting for about 80% to 90% of the causes. Cognitive decline identification aims to intervene early in secondary and reversible causes, as well as to plan the care of patients with dementia (SUS, 2017).
1 What is dementia? What are the physiological and psychological changes that occur for the older person with Dementia?
1.1 What is dementia?
Dementia is a disease characterized by slow and progressive loss of memory, concentration and learning ability, usually affecting people over 65 years of age. This disease may occur suddenly in young individuals when there is a serious injury, disease or due to certain toxic substances, such as carbon monoxide, responsible for destroying nerve cells. As a person ages, the brain changes generate a relative loss of memory, especially that of recent events, as well as a deterioration in learning ability. These changes do not affect normal functions. Lack of memory in older people is called benign senile memory loss, which does not necessarily mean that it is a sign of dementia or an early indication of Alzheimer’s disease (Marzanski, 2000).
1.2 Common types of dementia:
There are several types of dementia, and all share a common presentation of symptoms and are identified and classified based on the etiology. Some examples include: Dementia in Alzheimer’s Disease, Acute Onset Vascular Dementia, Multiple Infarct Dementia, Subcortical Vascular Dementia, Mixed Cortical and Subcortical Vascular Dementia, Dementia in Pick’s Disease, Dementia in Creutzfeldt-Jakob Disease, Dementia in Huntington’s Disease, Dementia in Parkinson’s disease, Dementia in disease caused by human immunodeficiency virus (HIV), Dementia due to neurosyphilis (Buchanan, et al., 2001).
1.3 Number of people with dementia in the world and Ireland
Every three seconds, a person is diagnosed with dementia in the world. Today, 47 million people suffer from this disease, but this number should be three times greater in 2050. Currently there are almost 55,000 people living with dementia in Ireland; 19,800 men and 35,650 women 4,000 of these people are under 65 and are classified as having younger onset dementia (Trépel, 2011). It is estimated that the number of people living with dementia will rise to 153,157 by 2046 due to population aging. Approximately 4,000 cases of dementia are identified in Ireland each year, there are approximately 50,000 family carers caring for someone with dementia for each person diagnosed with dementia there were at least three family members directly affected (Ireland, 2018).
1.3 Psychological changes
The psychological and behavioral symptoms of dementia are a term used to describe a variety of psychological and behavioral reactions that occur in people with dementia of any etiology. It can also be called non-cognitive aspects of dementia, since such terminology refers specifically to the behavior of the inherent subject to the symptom that causes pathologies. The psychological aspects of dementia constitute a psychopathological disorder other disorders of the third age and can be found in the varied etiological forms insanity. It ranges from psychotic symptoms (delusions and hallucinations), depression, insomnia, apathy and agitation, aggression, hypersexuality and wandering behavior.
In relation to the psychological aspects, the hallucinations produce changes of thought such as: Objects, people, animals and lights that do not fit into reality and that only the individual perceives. Delusions are mistaken beliefs, but held with great conviction and that usually manifests itself in dementia, we can use as an example: The delusions religious, megalomania, erotomania, paranoia and pathological jealousy. Depression is demonstrated by its apparent emotional aspect, one perceives sadness, anguish, dissatisfaction, lack pleasure in previously enjoyable activities, feelings of guilt and low self-esteem, there is also loss of energy and changes in sleep and appetite. Apathy is characterized by a lack of of initiative and indifference towards all aspects of life. The patient with this symptom refers more often to a certain neutrality about its own existence.
On the other hand, the behavioral aspects, such as agitation, the patient becomes restless, the every minute that he wanders, the patient of attention, commits himself physically because he/she has resistance to acceptance of care. In the aggression, it becomes hostile, being a danger to the physical and subjectivity and the collective, is prone to inadequate speech with clumsy language and Depreciative hypersexuality manifests itself in sexual behaviors (masturbation and display of genitalia), vocabulary with sexual connotation, attempted intercourse intense and fast sexual harassment.
Alzheimer’s disease presents all the symptoms mentioned above and this is therefore a general framework inherent in all forms of dementia. In addition, Alzheimer’s shows other symptoms that influence the individual’s life, such as ability to perform daily activities autonomously, which compromises the quality of life making it more and more dependent. Verbal behavior is deficient with difficulties find words, complete ideas or even follow instructions.
The thinking becomes obscure, forgetting, disorganized ideas, difficulty in learning new things, relationships with new experiences, reading and writing are outdated. In its most severe condition, the need for permanent patient care is generated by without motor control, fecal and urinary incontinence. In this sense, Alzheimer’s develops several psychosocial factors that only the life of the individual, but also of the family, leading to fatigue, anxiety, emotional and psychological stress for the limbs (Cerejeira, et al., 2012).
1.3 Physiological changes
The physiology of aging shows how the progressive decline of all the physiological processes of the human body occurs. Its purpose is to study the biological, physiological and anatomical variations and changes that the human being suffers over the years. Aging can be different from one individual to another. It is an individual process that fulfills its own rhythm, being gradual for some and faster for others. In it, there are many factors influencing, such as genetic load, lifestyle, socioeconomic conditions and chronic diseases.
Aging is a natural physiological process; however, it is possible to delay it from advances provided by science and preventive medicine. Physiological aging affects all human beings. It is characterized as a dynamic, progressive and irreversible process. In addition, it is a highly individualized process, which presents many differences between the subjects and between the associated functions, both biologically, psychologically and culturally. Its definition can be understood from three phases. Primary Aging: Primary aging is also known as “normal aging or senescence.” It reaches the body gradually and progressively, presenting cumulative effect.
We can say that senescence is a metabolic process of aging at the cellular level. To best exemplify, over time senescence cells lose proliferative capacity after a given number of divisions. Secondary Aging: Secondary or pathological aging is linked to the effect of disease and the environment on the body. It can be reversible or the target of a preventive intervention, for example: changes in the habits of life. Tertiary Aging: Associated with physical and cognitive losses.
It usually manifests itself in the advanced stage of old age. In addition, it presents rapid and abrupt decline, with deficiencies in the biological, immunological and psychological systems. Within the human aging process, there are some reduced physiological changes and capacities hearing capacity is reduced from 75 years of age.
Morphologically the tympanum tends to become thicker with age visual ability is reduced with greater difficulty in focusing on nearby objects and adapting to different brightness. Reduced taste capacity is observed with decreased taste, it also has a decrease in the production of saliva and a tendency to loss of teeth. Among the main physiological changes, we can also highlight the reduction of total body water (from 70% in children to 52% in the elderly), decrease in weight and height, changes in skin (senile stains, decrease in elastic fibers) and muscle tone, decreased respiratory capacity, cardiovascular and renal problems, among others.
These physiological changes are cumulative and progressively reduce the functional reserve of the individual. In this sense, there is a compromise of adaptive capacities and thus the individual becomes more susceptible to the development of diseases, functional reduction varies from person to person and from organ to organ (Nigam, et al., 2012).
2 Explore the person needs in relation to the condition
2.1 Maslow Hierarchy of Needs
Maslow’s famous hierarchy of needs, proposed by the American psychologist Abraham H. Maslow, is based on the idea that every human being strives hard to meet his personal and professional needs. It is a scheme that presents a hierarchical division in which the needs considered of lower level must be satisfied before the needs of higher level. According to this theory, each individual has to perform a hierarchical “escalation” of needs to achieve his full self-realization. For this, Maslow defined a series of five needs of being, arranged in the pyramid below and explained one by one:
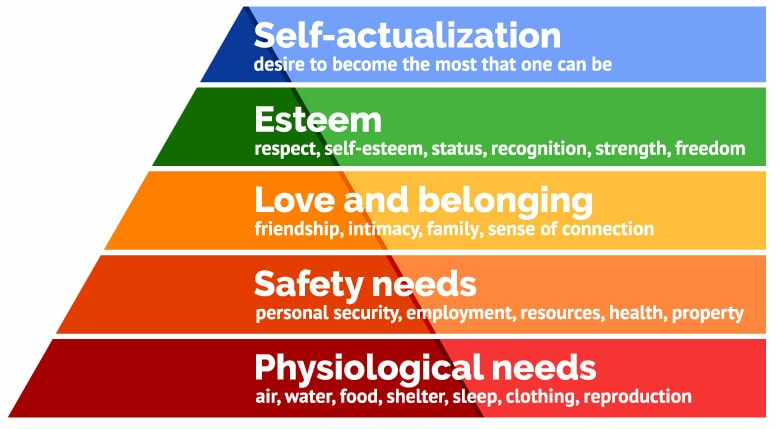 Figure 1- Maslow Hierarchy Needs
Figure 1- Maslow Hierarchy Needs
Where there are the primary (basic) needs that are the physiological and the safety needs and the secondary needs, which are the social, esteem and self-realization. Below is an explanation of each one:
2.2 Physiological needs
They are those that relate to the human being as a biological being. The most important are: the need to stay alive, to breathe, to eat, to rest, to drink, to sleep, to have sex, etc. At work: Need flexible hours, physical comfort, work intervals etc.
2.2 Safety needs:
Are those that are linked to the need to feel safe: without danger, orderly, safely, to save jobs, etc. At work: stable employment, health insurance, life insurance, etc. At work: Need for job stability, good pay, safe working conditions, etc.
2.3 Social needs:
They need to maintain human relationships with harmony: to feel part of a group, to be a member of a club, to receive affection and affection from family members, friends and people of the opposite sex. At work: Need to win friendships, maintain good relationships, have superiors, etc.
2.4 Needs of esteem:
There are two types: the recognition of our abilities for ourselves and the recognition of others of our capacity for adequacy. In general it is the need to feel dignified, respected by you and by others, with prestige and recognition, power, pride, and so on. Self-esteem needs are also included. At work: Responsibility for results, recognition by all, promotions throughout the career, feedback etc.
2.5 Self-realization needs:
Also known as growth needs. They include achievement, harnessing all of one’s potential, being what one can be, doing what one likes and is able to achieve. Relates to the needs of esteem: autonomy, independence and self-control. At work: Challenges at work, need to influence decisions, autonomy, etc (Lester, 2013)
3 What is the role of the carer and multidisciplinary team in assisting the person with dementia, what practices need to be implemented, what care settings are available?
The multiprofessional team plays a fundamental role in the orientation of the family, institutional caregiver or contracted because it is the team’s role to guide patients and family members about appropriate care with to patient and caregiver health quality standards. Thus, as health educators, professionals should also offer subsidies lay caregivers to choose the alternatives during the care they take without this function harming their health. In this context, the caregiver and the family are fundamental for the care of elderly people with Alzheimer’s disease in the home environment.
Whereas in its majority of the family members are neither physically prepared nor psychologically to live and take care of these older people, access to information on pathology and how to develop home care, which requires the follow-up of a multiprofessional team to provide the support and guidance from the implementation of programs with groups to support family members who take on the role of caring of the elderly with Alzheimer’s disease.
The multiprofessional team has the role of facilitating transmission of diagnosis, acceptance of treatments, relief of side effects, changes positive results in the patient’s lifestyle and his family, in addition to the professional approach with the social and emotional aspects of the patient, enabling a practical learning about the integrity and humanization of care. The diagnosis of Alzheimer’s disease for the family it is a moment of impact in the face of reality which highlights the need to tackle a new family situation (Australia, 2018).
Thereafter, they arise for the family caregiver difficulties such as loneliness, and, often, the lack of the necessary support of the other members of the family. With the support of health professionals, caregivers get to live better with their limitations in the care of the elderly with Alzheimer’s disease, group of caregivers, it is possible to share experi-difficulties, fears and conflicts with people who live similar situations.
The care of a person with dementia is important to their emotional well-being. However, people with Dementia generally are not able to start activities or entertain themselves. Here are some suggestions that may be helpful:
3.1 Develop a flexible attitude:
Everyone has days when feel very or very low energy and your friend or family member may be tired the day you visit. When things do not go as planned, remember that your visit continues to be important, both for you and the person you are visiting .
3.2 Be gentle with yourself:
Visiting a person with Dementia can sometimes be sad and difficult, so you may need support. Maybe you can take a supportive friend with you or plan to do something nice for yourself on the way home.
3.3 Take something with you:
It can stimulate the involvement of the person you are visiting, taking with you a magazine or newspaper. Together, you can read interesting articles or take a quiz. Carry flowers, candy or old photographs / postcards. These can become an activity that helps stimulation and reminiscence.
3.4 Establish a visitation ritual:
On all visits, say and do the same things on arrival and departure. This will help your relative or friend. Introduce yourself upon arrival. For example, say, “Hi, Mom, it’s me, Elisabete, your daughter.” Remembering your name and your kinship reduces the anxiety of your friend or relative. Do not make him guess.
3.5 Write letters and postcards:
Write together a letter to an ordinary or family friend. This can promote and maintain important connections in the person’s life with Dementia.
3.6 Introduce yourself to the team:
If you visit a residential care unit, introduce yourself and report your degree of relationship to the person you are visiting.
3.7 Silence is not a negative thing:
Try to learn to enjoy the moments of tranquility.
3.8 Provide a drink:
Will a cup of coffee, tea, or a glass of water help your friend or family member drink liquids, socialize, and keep the “old ones”? standards of hospitality.
3.9 Talking is not everything:
Embrace, massage hands and neck and shake hands, can replace or complement the conversation.
3.10 Start making a book of important things to remember:
This can be written and read by all visitors and function as a stimulant of the memory of your friend or relative.
3.11 Make a book of life:
This is a great way to validate the life of your friend or family member and remember ancient deeds. Build it during the visits. This project can make your time together even more enjoyable and special.
3.12 Consider performing tasks:
Sew labels on clothing, help at mealtimes, or take the person you are visiting for a walk. This in addition to benefiting the person, will maintain their vital role and help you feel useful and important. It will also assist the team of the residential unit.
3.13 Play an instrument or sing:
If you are a musician, consider playing an instrument or singing to your friend or family member. The music promotes relaxation, the return of pleasant memories and feelings of tranquility and security.
3.14 Carry an animal or your pet with you:
Visiting a beloved pet can improve the emotional health and well-being of your friend or relative. If the visit takes place in a residential home, talk to the team before taking the animal with you.
3.15 Know that your visit makes a difference:
People who live in residential homes need emotional support for their well-being and when they have regular weekly visits they are less likely to be depressed.
3.16 If necessary, talk to someone:
There are many issues around changing roles and the sadness that affects the families, friends, and caregivers of people with Dementia. It is very important to take care of yourself (Monahan, 1993).
Conclusion
4 State the current approaches towars developing quality services for people with dementia.
According to ADI (2013) the National Dementia Plans are the most powerful tool in transformation of national dementia support and treatment. Plans help governments to ensure that social and health care systems are well structured and adequately funded to ensure high quality support and treatment available to people living with dementia today and in the future. According to the same report, in October 2013, 19 countries had national strategies outlined for the insanity. Since some of the plans are already in their 3rd edition, which means that they were implemented, evaluated and updated.
For the construction of this framework, all the National Plans for the found in English. After this selection a according to the criteria proposed by Alzheimer Disesase International (ADI). National Plans for dementia raise awareness of stigma reduction; specific training in dementia for health care professionals and family caregivers and timely access to diagnosis and treatment. Access to diagnosis is particularly relevant in view of the account that, overall, people are under-diagnosed., (Alzheimer’s Disease International, 2015)
There are few countries that do not explicit the care philosophy that informs the plan and almost all, in a more or less explicit way, present the Person-Centered Approach with dementia as the following resolutions: Resolution nº133 / 2010 – Recommends recognition of dementia as a national priority and the creation of a National Dementia Program. Resolution 134/2010 – Recommends that the dementia approach be considered priority, a national intervention plan for dementias and necessary measures to provide adequate support to patients and their families (Davison, et al., 2012).
References
-
Australia, D., 2018. Dementia Australia. [Online]
Available at: https://www.dementia.org.au/
[Acesso em 07 January 2019]. - Buchanan, R. J., Wang, S. & Huang, C., 2001. Analyses of nursing home residents with HIV and dementia using the minimum data set.. Journal of Acquired Immune Deficiency Syndromes, , 26(3), pp. 246-255.
- Cerejeira, J., Lagarto, L. & Mukaetova-Ladinska, E. B., 2012. Behavioral and Psychological Symptoms of Dementia. Frontiers in Neurology, , 3(), pp. 73-73.
- Davison, T. E. et al., 2012. An evaluation of a national program to implement the Cornell Scale for Depression in Dementia into routine practice in aged care facilities.. International Psychogeriatrics, , 24(4), pp. 631-641.
-
Ireland, T. A. S. o., 2018. Information for the Media. [Online]
Available at: https://www.alzheimer.ie/About-Us/News-and-Media.aspx
[Acesso em 07 January 2019]. - Lester, D., 2013. Measuring Maslow’s Hierarchy of Needs. Psychological Reports, , 113(1), pp. 15-17.
- Marzanski, M., 2000. On telling the truth to patients with dementia. Western Journal of Medicine, , 173(5), pp. 318-323.
- Monahan, D. J., 1993. Assessment of Dementia Patients and their Families: An Ecological-Family-Centered Approach. Health & Social Work, , 18(2), pp. 123-131.
- Nigam, Y., Knight, J., Bhattacharya, S. & Bayer, A., 2012. Physiological Changes Associated with Aging and Immobility. Journal of Aging Research, , 2012(), pp. 1-2.
- SUS, 2017. Clinical Review – Dementia. RegulaSus, 1(1), p. 11.
- Trépel, D., 2011. Informal Cost of Dementia Care – A Proxy-Good Valuation in Ireland. Economic and Social Review, , 42(4), pp. 479-503.
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allDMCA / Removal Request
If you are the original writer of this essay and no longer wish to have your work published on UKEssays.com then please click the following link to email our support team:
Request essay removal


