What Effect Does Combining Clozapine with Second-generation Anti-psychotics Have in Reducing Symptoms in Schizophrenia?
Info: 9184 words (37 pages) Dissertation
Published: 11th Dec 2019
Tagged: MedicalPsychology
Rationale and Aims: 4, 788 words
This review seeks to answer; what effect does combining Clozapine with second-generation anti-psychotics have in reducing positive and negative symptoms in people with Schizophrenia? By critically analysing five papers, one will aim to conclude on the efficacity of combining clozapine with other antipsychotic medication to reduce one’s symptoms.
Inadequate responses to Clozapine treatment are frequently encountered in clinical practice and augmentation strategies have therefore been developed to try and improve this. One idea for an intervention may be by adding a second-generation antipsychotic to explore whether this treatment has any significant benefits for people or whether it acts as a placebo effect instead (Galling et al., 2017).
Approximately 25% of adults living within the UK, suffer from mental health illnesses (Mind, 2013a). With Schizophrenia being prevalent amongst men and women, most are diagnosed between the ages of 18- 35 years. However, there are issues surrounding treatment options for people whom an anti-psychotic has had little or no effect.
For people who have been diagnosed with treatment resistant Schizophrenia and who’s illness has not responded sufficiently to clozapine at an enhanced dose, healthcare professionals should be measuring therapeutic blood levels, before adding a second antipsychotic to combine treatment with clozapine. Having said this an adequate trial of combinations would need to be at least 8–10 weeks. NICE (2009) suggests that when choosing another drug to combine, considerations as to the composites should be taken into account, this is to not compromise the common side effects of Clozapine (NICE, 2014) (1.5.7.3).
Literature review aims
- Explore current literature on augmentation of clozapine with a second-generation antipsychotic.
- Explore policies and national guidelines to support my research.
- Evidence to support that adding a second-generation antipsychotic or use of a long acting antipsychotic injection reduces symptoms.
- Promote multi-agency working to produce effective outcomes to elevate suffering.
Literature search strategy and structure for my review.
The search terms for this review were derived from the following PICO template (Scala, Price and Day, 2016). Using a wide range of data bases such as Ebasco, PubMed, and Cinahal. The terms entered were (P)” Clozapine patients”AND” “service users/clients” (I) “Schizophrenia” AND “second generation anti-psychotic” (C) “Effectiveness” OR “Efficacy in patients in Schizophrenia” “in conjunction with other antipsychotics (O) “reduction in symptoms” AND “positive and negative symptoms” AND “improvement”. Databases searched conjointly in March 2017 via PRIMO include; AMED (EBSCO), Psych INFO, Schizophrenia bulletin, PubMed, MEDLINE (EBASCO), and The Cochrane Library along with NICE guidelines.
Initial search terms that limited the title were “Clozapine” AND “additional anti-psychotic” which produced (640 hits). This included Cipriani, Boso and Barbui, (2009) and Lewis et al (2006). “Augmentation” OR “trials of at least two second generation anti-psychotic drugs with poor clinical response” AND “Schizophrenia”, including “all” were searched for, producing (145 hits) including Galling et al (2017) and Muscatello et al (2011) The Schizophrenia bulletin was searched using the best terms “Schizophrenia” “Clozapine” AND “augmentation” OR “combination strategies”, limited to all topics, not including “a history of neuroleptic malignant syndrome” OR “ physical health issues” (13 Hits) Freudenreich et al (2007) Five papers were found for analysis:
One paper was a Randomised control trial (RCT) and is known as the (gold standard) of evidence, recently coming second only to systematic reviews (Evans, 2003). Another two papers collected were systematic reviews. A systematic review aims to collect as much relevant research on a certain topic, then critically analysis several papers and synthesis research results in a way that makes it easier to use the results to form decisions in practice (Ccace.ed.ac.uk, 2013). The Fourth paper was a longitudinal qualitative study which is designed to study people over several years, it is purely qualitative, however, quantitative methodology is limited due to hypothetical evidence yet, having said this, it does provide a valuable perspective (Shuttleworth, 2009). The fifth and final paper reviewed is a quantitative study incorporating a double blinded, parallel trial. A parallel trial aims to reduce bias, due to the randomisation process, ensuring that results are accurate and bias is reduced (REF).
Papers which were not relevant, were disregarded due to not relating to the search question or being duplicate hits. The papers that were automatically included were if they sought to explore the effectiveness of Clozapine augmentation with a second-generation antipsychotic or if they had previously built on research in this area. The Cochrane Library of systematic reviews (2014).
Critical appraisal of body of literature 1,750 words
The literature will be critically appraised using the Critical Appraisal Skills Programme Critical Appraisal Skills Programme (CASP) (2013).
The papers in this review will initially comprise of quantitative studies and aims to quantify numerical data through the process of systematically testing which allowed for a relationship to be hypothesised between variables. An independent variable exposed to certain conditions and dependent variables sought to explore how the quality was affected by the intervention, subsequently, results were established or otherwise disregarded (McLeod, 2008).
To ensure internal validity, causes of systematic basis within study designs must be acknowledged and organised, otherwise this can lead to a misinterpretation of results found, resulting in errors of inference (Socialresearchmethods.net, 2006)
Lewis et al., (2006) undertook a quantitative randomised control trial of Clozapine vs. other second generation antipsychotics (SGA) for schizophrenia with a blind rating outcome over the course of one year. The aim of their research was to determine the efficacy of Clozapine and a SGA combined in reducing symptoms and lower heath costs.
Inclusion criteria was defined to a DSM-IV Schizophrenia diagnoses in patients that were eighteen to sixty-five years of age and have had a poor response rate to at least two previous anti-psychotics (Ref). Exclusion criteria was distinguished by excluding people with substance misuse or a medical disorder along with a history of neuroleptic malignant syndrome. Primary outcome measures were scored using the Quality of Life Score (QLS) (Bobes et al., 2005). whist secondary measures were used in line with the Positive and Negative syndrome scale (PANNS) (Mortimer, 2007). A total of 168 participants were initially referred by clinicians, however 32 were not randomised due to not meeting the inclusion criteria. Of the 136 patients, (n= 67) were randomly assigned to receive Clozapine and (n=69) were randomly assigned to receive the SGA.
The trial was rater-blind in nature, which included the physical location of assessors combined with a system of passwords and randomisation lists which incorporated an encrypted email from the randomisation centre. Participants were also reminded not to discuss treatment assignments. An intention to treat effect was present, exploring analytical factors and ensuring balance between treatment groups. The methodology behind using an intention to treat method was to provide an estimate as to how many participants would benefit from this treatment; it also looks at the clinical benefits and the cost effectiveness of delivering the combination (Williamson and Whittaker, 2014).
There appears to be an element of detection bias present within this study as one assessor found out another drug a patient was currently receiving (ref). Attrition bias was also present due to the number of patients (7%) withdrawing from the study early or were lost to follow up, consequently, elements of data were lost leading to internal validity. Having said this, the mean dosage of Clozapine was relatively low with target ranges for dosages being between 200 to 450mg a day which is a relatively low dose (Evidence.nhs.uk, 2014).
Overall, this study is comparatively small, however, it does provide sufficient information into primary outcome measurements, with results showing that Clozapine is an effective intervention if combined with a SGA to improve positive and negative symptoms of Schizophrenia despite the detection of bias’s outlined. 430 words
Moving on to Gailing et al, (2017),whoundertook a systematic review and meta-analysis of randomised trials comparing augmentation with a SGA vs continued anti-psychotic use. Participants included at least twenty people with a diagnosis of schizophrenia who were assigned to augmentation therapy with the aim to reduce symptoms, which were assessed against a [PANNS] scale (Anderson,1984 in Gailing et al, 2017).
Strengths of this paper included randomization of participants to the medication that they were to receive. However, it can be argued as to how the randomisation process took place or what process was involved as this was not explained in this paper, indicating an element of selection bias. Contrastingly, this paper was a study undertaken in China that failed to assess the reduction rate of symptoms because there was not enough data to support findings, thus, reducing its generalisability to other populations (Gailing et al, 2017).
A study of heterogeneity was explored utilising I2 > 50% with a P. value of 0.05 indicating significant heterogeneity. A Chi-Square test was also utilised as a measuring tool. An advantage of using a Chi-square test is that it is used to compare variables at a nominal level and is used in quantitative research because of its robustness in respect of distributing data with ease as well as handling data from multiple group sizes as outlined in this study (McHugh, 2013). Stratified random sampling was also used to determine the subgroups of the population used and was identified to reflect some characteristics such as gender and sex (Reference), nevertheless, the paper cannot disregard selection bias, amongst patients who were not severely ill.
Furthermore, patient’s adherence rate to the medication they were taking was not measured effectively as participants could have been dishonest about taking their medication compliantly. Perhaps, the biggest sources of bias outlined in the paper comes from the blinding and intention to treat (ITT) category because it is unclear that comparisons between treatments would be clinically effective (Ref).
This research compares augmentation vs continued usage of an anti-psychotic; therefore, the results of this study are limited in the fact that participants were not specified to be male or female, baseline measurements were not taken beforehand and internal validity appears to be a concurrent theme throughout. The study used a small number of double blind studies, with some not reporting the adverse effects which limits external validity and the number of patients who completed the treatment (Reference). 380 words
Cipriani, Boso and Barbui, (2009)’s study sought to determine whether the efficacy and tolerability of various Clozapine strategies with anti-psychotics would improve symptoms for people with treatment resistant schizophrenia. The study only included RCTs of people who were eighteen years and older and had diagnoses of treatment resistant Schizophrenia already in place, comparing Clozapine plus an additional anti-psychotic drug.
In an RCT patients are randomised, by chance into two groups. One of these is a test group (Intervention) the other is a control group (participants not receiving any intervention) this is to ensure homogeneity allows for a fair comparison (Medical Research Council, 2013). Twenty-four studies were looked at, however only three of these twenty-four fulfilled all the inclusion criteria, leaving a total of people randomised at one hundred and forty. These studies included Kong (2001), Gene (2007) and Zing (2008).
It can be argued, both Kong’s (2001) and Gene’s (2007) RCTs used an inadequate method of randomisation and allocation, due to the lack of reporting, thus leaving both studies open to allocation bias, through lack of concealment. However, in Zing’s (2008) study, it was reported that randomisation occurred using a biometrician and numbers being generated at random, yet failed to report on how participants were allocated to the study. Consequently, all three trials fail to report any information on how participants were allocated to their trials indicating that allocation bias was present in all (Day, 2000).
Gene (2008) was an open study, whereby only the rater remained blinded to the medication throughout the study. It is assumed, participants and providers were aware of the allocated treatment and thus, lead to performance bias and subsequent observational bias could have resulted in differences that occurred (Jolley, 2013).
Higgins (2008) suggests, because of the small sample of people being studied the results may yield misleading. This is thought to be because the lower the sample, the higher the risk of discrepancies between treatment groups could potentially occur. Therefore, to conclude, this paper has identified flaws in the form of allocation concealment and lack of reporting thus, it was unable to generalise results over which antipsychotic would work better in terms of being combined with Clozapine to elevate positive and negative symptoms in patients. 358 words
Muscatello, et al (2011) carried out a longitudinal qualitative study into the introduction of Aripiprazole in conjunction with Clozapine in Italy, which comprised of forty outpatients including male and females, who had met the diagnostic criteria from the DSM-V on Schizophrenia. Patients included demonstrated that they had been having persistent positive and negative symptoms even though they have already been commenced on Clozapine previously.
Aripiprazole in combination with Clozapine has been described in case reports, however, RCT evidence remains limited (Chang et al, 2008). In a twenty-four week, double blinded and randomized placebo trial patients with a diagnosis of Schizophrenia were given either a placebo or Aripiprazole. Baseline measurements were taken before the study commenced and measured using a Scale for the Assessment of Negative Symptoms [SANNS] and a Clinical Global Impression Improvement Scale [CGI-I].
The dependent variable identified in this study is the PANSS scale used to measure the severity of symptoms that people have been experiencing. The independent variable being identified as people who have a diagnosis of Schizophrenia and are currently taking Clozapine. However, results cannot be generalised because Inter-rater reliability was not established throughout, thus making the consistency between observers unreliable (Ref).
According to Kottner et al., (2011) inter rater reliability is the agreement of the same data, which is collected by different raters using the same scales; data that has been found from findings has to be consistent. Conversely, scales and measuring devices come in many different forms, therefore, categories need to be outlined beforehand because raters could have different interpretations of wording in clinical interviews.
A type 1 error was also present in this study and is based on the researcher’s rejection of the null hypothesis when it is true (Ref). The study took this into account when assessing efficiency ratings and as a method to reduce the potential for type 1 errors a Bonferroni correction was applied. A Bonferroni correction is a non-parametric measure used to test for significance in a study (Ref), with another analysis method of Variance [ANOVA] being used to determine if one method was better than another.
However, the study is based on a small sample size, hence compromising the reliability of results: Thirty-one participants completed the study, with nine dropouts Bell, et al (2013) argues that bias may not always occur and is dependent on what analyse methods are used, furthermore, the dropout rate is something that is a frequent occurrence in longitudinal studies due to follow ups not being carried out.
Lastly, Freudenreich et al (2007)’s study sought to examine if Risperidone was added to stable, yet, symptomatic patients who are already commenced on Clozapine, would this combination reduce symptoms and improve a patient’s overall psychopathology?
A double-blind placebo controlled parallel group was used in twenty-four outpatients, with a dose of 4mg/daily of Risperidone added for approximately six weeks to patients who have a current diagnosis of Schizophrenia. An advantage of using a parallel group method is that participants are randomised, this is to ensure accuracy of results and limit the risk of bias occurring. (REF)
Parahoo (2009) states that being aware of which interventions the control and the experimental groups are receiving could potentially introduce bias on behalf of the researchers, he goes on further to suggest that it is important to avoid this type of influence especially if both drugs look similar and not let participants know what group they are currently assigned to. Scaling systems such as PANNS were used, accompanied by the SANNS to asses if there was an improvement in patient’s symptoms.
Clinical variables were analysed using a linear regression model, seeking to explain the relationship that exists between variables, in this case a change in PANSS score is the dependent variable and medication as the independent variable.
Of the one hundred and twenty-three Clozapine participants’ fifty-six (45%) declined to take part, along with thirty-nine patients (32%) who were not eligible to take part in the study because they were already receiving antipsychotic polypharmacy, therefore, this left only twenty- eight participants (23%) who had agreed to participate fully.
A disadvantage to this study comes in the form of the randomisation process, unlike Gailing’s et al, (2017) study, this paper states that participants were randomised to either receive Risperidone or a placebo, however, it fails to state as to how the randomisation process occurred, leaving the study open to attrition bias and allocation bias. Additionally, the sample size was reduced from n= 56 to n= 28 weakening the generalisability of their findings (Macnee and McCabe, 2008).
Synthesis 500 words
Randomised control trials tend to represent the “gold standard” of research designs, coming second only to systematic reviews in the hierarchy of evidence. The position of the study designs is based on their rigour (Ref). The designs most vulnerable to bias are believed to be less clinically significant and are placed at the bottom of the hierarchy (Ref) however, one must appraise the evidence to deem where it stands in terms of clinical importance and the suitability in regards to answering the research question that is being asked (Ref).
In partially responsive Schizophrenia patients, The National Institute for Health and Care Excellence [Nice] guidelines have made recommendations into introducing a second antipsychotic to patients who are already receiving Clozapine to see if this will elevate some of the crippling symptoms that patients experience (NICE, 2014). It has also been discussed as to the potential benefit it could have in the reduction of positive and negative symptoms that are associated with the condition. Having said this, Cipriani et al (2010) argues that there is still much debate as to which antipsychotic combination works more efficiently, with no new evidence signifying that one antipsychotic is inferior of another or has a lesser side effect profile. Additionally, combination strategies are a suggested option in the Maudsley prescribing guidelines in patients who have long term compliance problems (Taylor et al., 2015 in Souaiby, et al, 2017).
The overall results from the five papers chosen all follow a similar pattern, this is that because of the small sample sizes being used to measure the effectiveness of Clozapine in combination with other antipsychotics, research remains limited and somewhat outdated, with little or incomplete research determining which antipsychotic would give the best results and reduce symptoms.
By using a PANNS and SANNS scaling system to assess patient’s symptoms, it allows for a balanced representation of the positive and negative symptoms and both are considered valid in assessing the extent of the severity one’s illness impacts on one’s life. It also severs to measure their relationship to one another. Nonetheless, both differ due to not taking into consideration integration of global scores and differences in domain coverage along with the extensively systematized interviews (Daniel, 2013).
Therefore, results cannot be generalised to a population without using bigger trials and more case studies being needed to measure the extent of whether Clozapine in conjunction with another second-generation anti-psychotic would indeed benefit Schizophrenia patients or outline which anti-psychotic would be beneficial to patients in respect of showing a reduction in symptoms or adverse side effects. Secondly, variables need to be clearly defined and more effective trials need to be undertaken with the use of randomisation being applied along with an intention to treat analysis also being applied to reduce any potential bias. Although, the studies included have tried to exclude bias, no study will be completely free, this is due to a multitude of factors ranging from loss of participants to follow up and noncompliance, which in turn, leaves results statically reduced (ref).
The Intention to treat (ITT) principle is important and should be applied in research if it is appropriate to do so, because it aims to reduce bias by providing an estimate in terms of the effect on treatment outcomes (Shrier, et al, 2014). With the method of “once analysed, always randomised” being applied. An advantage of using the ITT principle is that it admits to non-compliance rates and protocol deviations (Gupta, 2011). Furthermore, it does try to minimise type 1 errors allowing for the best results in terms of generalizability.
Nevertheless, ITT cannot always be applied, another method that could be used instead of ITT is a Per Protocol [PP] analysis, which aims to exclude participants who did not complete that treatment or have switched groups, thus, PP is most likely to give an understanding of the efficacy of treatment under the best conditions (Sainani, 2010).
Despite this alternative analysis, PP provides a weaker level of evidence and makes things look different, therefore, an ITT method would be more appropriate due to it guarding against potential bias and preserves randomisation, keeping groups as equal as possible to prognostic factors to see what effect the intervention has on the outcome, which in turn gives a higher level of evidence intended for clinical treatments. 636 words
Research Proposal
State my research questions and hypothesis Aims and Objectives 250 words
Although Clozapine adjunctive’s have shown to be beneficial in people who suffer from Schizophrenia, Clozapine combination outcomes remain poor. Sommer et al, (2011) suggests that between one-fifth to one third of patients have limited benefit, furthermore, treatment- resistant patients often remain highly symptomatic which in turn, equals lengthier periods of hospitalization, equating to more expense to national health services.
Schizophrenia is a chronic disorder, which is characterised by repeated relapse, that can lead to severe consequences for patients and their quality of life, this includes their psychosocial functioning along with the financial responsibility for patient’s families, this is because patients may not return to their previous levels of functioning after subsequent relapses (.
In 2009 the Schizophrenia patient’s outcomes research team conversed around the efficacy of adjunctive treatment, however, the research team argue that due to the failed documentation of efficacy and patients showing limited signs of improvement in using the combined treatments, along with the appropriate rating scales being in situ, research still remains limited, this is in respect of making suitable recommendations that can support patients suffering from Schizophrenia. 181 words
Methodology 750 words
This research aims to determine the efficacy of using Clozapine in conjunction with a long acting second generation antipsychotic injection such as Aripiprazole rather than an oral antipsychotic to assist in elevating an individual’s symptoms which will be assessed using a quality of life scale [QLS] and positive and negative symptom scale [PANNS] to measure outcomes, it is also looking to manage a patient’s concordance rate better and gives people in the community the option to utilise this also.
Parahoo (2006) states that quantitative designs use statistical and numerical data, seeking to investigate the association and possible links between variable’s. Due to wanting to explore the efficacy of using a long acting anti-psychotic depot such as Aripiprazole further, an experimental quantitative strategy will be employed to undertake this research proposal.
The underlying philosophy of quantitative research comes from a positivist approach. Positivism argues that traditional methods of scientific techniques are an appropriate intervention into studying society, this is because of the fixed laws incorporating the cause and effect with sampling playing an important part, placing a greater emphasis on creating generalisations that are statistically significant and that can be applied to a population (Robson, 2008 in Williamson and Whittaker, 2014). Payne and Payne, (2004) states that critics have challenged some of the core assumptions put forward from a positivist approach which in tow has led to a more sophisticated adaption of the traditional scientific approach being referred to as realism.
To explore this further, a Randomised Control Trial [RCT] would be needed, with considerations to relevant variables such as environment, stage of illness and the setting, also considering what patient population one would be intending to treat, i.e inpatients would be more suitable as the trial would need to take place in a controlled environment with the facilities to undertake the specific monitoring that would be associated. Baseline observations and blood levels would firstly need to be taken with outcome measurements being assessed using a PANNS and QLS scale. Follow up measures will also take place at 6,12 and 28 weeks. 325 words
Methods 1,000 word
According to Lally et al, (2016) Clozapine is the only evidence based treatment for treatment resistant Schizophrenia [TRS], with approximately 60-70% of people showing a response, although this figure varies depending on a setting and patient population. However, for people who are non-responsive, despite acceptable blood levels there is the option to use a long acting anti-psychotic injection, this is dependent on patient’s tolerability of medication and whether this will be a more suitable option to taking oral medication in respect of historical concordance rates.
Sampling method Quality of life and symptomatic improvements.
Side effect profile
Inclusion and exclusion criteria is outlined in Text box 2
Inclusion Criteria
- People who have ongoing psychosis.
- People who are 18 to 60 year’s old.
- People who have tried adequate doses of at least two anti-psychotics, one of which is a non-Clozapine second generation anti-psychotic (NICE Guidelines, 2009).
- Lack of adherence.
Exclusion Criteria
- People who lack capacity to consent to treatment.
- People younger than 18 years of age.
- People who have a history of neuroleptic malignant syndrome or substance misuse.
- Previous treatment with long acting antipsychotics within 6 months prior to screening.
Nice.org.uk (2014) states that before introducing any long acting antipsychotic injection, one must consider patient’s preferences and attitudes towards the mode of administration and think about where the most appropriate setting would be, i.e clinical location such as a hospital or clinical room.
A registered Nurse will be responsible for taking and monitoring patients vital signs and baseline observations such as systolic and diastolic blood pressure readings, temperature and blood tests indicating red, amber or green light: (see appendix 1) which will be done weekly for the first 18 weeks, then every 2 weeks for 1 year. An ECG will also be needed before patients are initiated on the combination treatment, due to the potential of tachycardia happening.
Dur, Harvey and Caceda (2017) suggest that by using Clozapine in combination with long acting injectable antipsychotics [LAI] have a distinct advantage over oral antipsychotics this is because the LAI is not influenced by first pass metabolism, which in tow reduces the likelihood of prospective drug to drug interactions. However, Agid, Fousisas and Remmington (2010) state that despite LAI’s having potential advantages, LAI are also not as widely used as one might expect, this could potentially be down to clinician’s own misconceptions surrounding the appropriateness of the combination and the fabrication of an increased side effect profile.
Patients will be asked to consent to this and asked about their smoking status also. Information is to be given to patients and carers about Clozapine combinations, including side effects that could potentially occur because of titration levels or changes in blood levels. One would also need to consider the longer-term side effect profile of combination treatment, paying attention to a patient’s life skills and their ability to function. Furthermore, under The Mental Capacity Act (2005) a patient has the right to withdraw from a research study at any time, their wishes must be respected (Gmc-uk.org, 2017).
495 words
Application to practice and Dissemination methods 250 words
This research is aimed at supporting Registered Mental Health Nurses and other clinicians in how best to approach Clozapine combination therapies including that of which a long acting antipsychotic would be more suitable for patients, this is in respect of treating and minimalizing some of the positive and negative symptoms patient’s experience, alongside managing relapse rates and increasing long term adherence to treatment.
It is also anticipated that this research could potentially assist clinicians to encourage patients to try other alternatives with Clozapine such as a long acting injection over oral medications due to ongoing- issues with concordance of medication and minimal side effect profiles, this would be using the best available evidence based practice to support decisions surrounding ongoing care and treatment.
Dissemination methods of this research will be completed in a published nursing journal (RCNi 2014). All participant’s that took part in the study will receive information in the form of a pamphlet as to the efficacy of combination therapies and which anti-psychotic combination showed the most improvement overall in reducing a patient’s symptoms, less side effects and tolerability.
A letter of acknowledgement and an expression of gratitude will also be included, which will contain confirmation that all data used for this study will be destroyed after dissemination of one’s research. 181 words
References
Agid, O., Foussias, G. and Remmington, G. (2010). Long-acting injectable antipsychotics in the treatment of schizophrenia: their role in relapse prevention: Expert Opinion on Pharmacotherapy: Vol 11, No 14. [online] Taylor and Francis Online. Available at: http://dx.doi.org/10.1517/14656566.2010.499125 [Accessed 20 Apr. 2017].
Barber, S., Olotu, U., Corsi, M. and Cipriani, A. (2017). Clozapine combined with different antipsychotic drugs for treatment-resistant schizophrenia. Cochrane Database of Systematic Reviews, [online] pp.8-13. Available at: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD006324.pub3/full [Accessed 26 Mar. 2017].
Bell, M., Kenward, M., Fairclough, D. and Horton, N. (2013). Differential dropout and bias in randomised controlled trials: when it matters and when it may not. BMJ, [online] 346(jan21 1), ppe8668-e8668. Available at: http://www.bmj.com/content/346/bmj.e8668 [Accessed 11 Apr. 2017].
Bleakley, S. and Henry, R. (2016). Clozapine: Guidelines for a red blood result. [online] Southernhealth.nhs.uk. Available at: http://www.southernhealth.nhs.uk/EasysiteWeb/getresource.axd?AssetID=77706&type=full&servicetype=Inline [Accessed 17 Apr. 2017].
Bobes, J., García-Portilla, P., Sáiz, P., Bascarán, T. and Bousoño, M. (2005). Quality of life measures in schizophrenia. European Psychiatry, [online] 20(3), pp.S313-S317. Available at: http://www.sciencedirect.com/science/article/pii/S0924933805801828 [Accessed 21 Mar. 2017]
Ccace.ed.ac.uk. (2013). Systematic reviews and meta-analyses: a step-by-step guide | www.ccace.ed.ac.uk. [online] Available at: http://www.ccace.ed.ac.uk/research/software-resources/systematic-reviews-and-meta-analyses [Accessed 10 Apr. 2017].
Cipriani, A., Boso, M. and Barbui, C. (2009). Clozapine combined with different antipsychotic drugs for treatment resistant schizophrenia. Cochrane Database of Systematic Reviews, [online] pp.8-13. Available at: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD006324.pub2/full [Accessed 24 Mar. 2017].
Critical Appraisal Skills Programme (CASP). (2017). Critical Appraisal Skills Programme (CASP). [online] Available at: http://www.casp-uk.net/appraising-the-evidence [Accessed 16 Mar. 2017].
Daniel, D. (2013). Issues in Selection of Instruments to Measure Negative Symptoms. [online] Schizophrenia Research. Available at: http://www.schres-journal.com/article/S0920-9964(13)00349-6/pdf [Accessed 22 Apr. 2017].
Day, S. (2000). Statistics Notes: Blinding in clinical trials and other studies. BMJ, [online] 321(7259), pp.504-504. Available at: http://www.bmj.com/content/321/7259/504 [Accessed 31 Mar. 2017].
Dur, D., Harvey, P. and Caceda, R. (2017). Comparison of pre-treatment clinical characteristics and post-treatment outcomes of patients treated with Clozapine and long acting antipsychotics. [online] Openaccessjournals.com. Available at: http://www.openaccessjournals.com/peer-review/comparison-of-pretreatment-clinical-characteristics-and-posttreatment-outcomes-of-patients-treated-with-clozapine-and-long-acting-.html#10 [Accessed 20 Apr. 2017].
Evans, D. (2003). Hierarchy of evidence: a framework for ranking evidence evaluating healthcare interventions. Journal of Clinical Nursing, [online] 12(1), pp.77-84. Available at: http://onlinelibrary.wiley.com/doi/10.1046/j.1365-2702.2003.00662.x/ful l [Accessed 26 Mar. 2017].
Evidence.nhs.uk. (2014). CLOZAPINE : British National Formulary. [online] Available at: https://www.evidence.nhs.uk/formulary/bnf/current/4-central-nervous-system/42-drugs-used-in-psychoses-and-related-disorders/421-antipsychotic-drugs/second-generation-antipsychotic-drugs/clozapine [Accessed 20 Mar. 2017].
Freudenreich, O., Henderson, D., Walsh, J., Culhane, M. and Goff, D. (2007). Risperidone augmentation for schizophrenia partially responsive to clozapine: A double-blind, placebo-controlled trial. [online] Science Direct. Available at: http://www.sciencedirect.com/science/article/pii/S0920996407000321 [Accessed 11 Mar. 2017].
Galling, B., Roldán, A., Hagi, K., Rietschel, L., Walyzada, F., Zheng, W., Cao, X., Xiang, Y., Zink, M., Kane, J., Nielsen, J., Leucht, S. and Correll, C. (2017). Antipsychotic augmentation vs. monotherapy in schizophrenia: systematic review, meta-analysis and meta-regression analysis. World Psychiatry, [online] 16(1), pp.77-89. Available at: http://onlinelibrary.wiley.com/doi/10.1002/wps.20387/epdf [Accessed 20 Mar. 2017].
Gmc-uk.org. (2017). GMC | Consent to research: Right to withdraw from research. [online] Available at: http://www.gmc-uk.org/guidance/ethical_guidance/6475.asp [Accessed 20 Apr. 2017].
Gupta, S. (2011). Intention-to-treat concept: A review. Perspectives in Clinical Research, [online] 2(3), p.109. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3159210/ [Accessed 15 Apr. 2017].
Jolley, J. (2013). Introducing research and evidence-based practice for nursing and healthcare professionals. 1st ed. Harlow: Pearson, p.126.
Kottner, J., Audige, L., Brorson, S., Donner, A., Gajewski, B., Hróbjartsson, A., Roberts, C., Shoukri, M. and Streiner, D. (2011). Guidelines for Reporting Reliability and Agreement Studies (GRRAS) were proposed. [online] Elsevier. Available at: http://ac.els-cdn.com/S0020748911000368/1-s2.0-S0020748911000368-main.pdf?_tid=05234c5e-1700-11e7-bba2-00000aab0f01&acdnat=1491067631_1563b3aa92d6620b12605dba2fd97b80 [Accessed 1 Apr. 2017].
Lally, J., Gaughran, F., Timms, P. and Curran, S. (2016). Treatment-resistant schizophrenia: current insights on the pharmacogenomics of antipsychotics. Pharmacogenomics and Personalized Medicine, [online] Volume 9, pp.117-129. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5106233/ [Accessed 17 Apr. 2017].
Lewis, S., Barnes, T., Davies, L., Murray, R., Dunn, G., Hayhurst, K., Markwick, A., Lloyd, H. and Jones, P. (2005). Randomized Controlled Trial of Effect of Prescription of Clozapine Versus Other Second-Generation Antipsychotic Drugs in Resistant Schizophrenia. Schizophrenia Bulletin, [online] 32(4), pp.715-723. Available at: https://academic.oup.com/schizophreniabulletin/article/32/4/715/1934800/Randomized-Controlled-Trial-of-Effect-of [Accessed 18 Mar. 2017].
McLeod, S. (2008). Dependent Variable – Independent Variable | Simply Psychology. [online] Simplypsychology.org. Available at: https://simplypsychology.org/variables.html [Accessed 11 Apr. 2017].
Medical Research Council (2012) Gold standard: What are Randomised Control Trials and Why Are They Important? [online] Available at: https://www.youtube.com/watch?v=U6kVIRn6G0w [Acssesed 21 Mar. 2017].
Mind.org (2013a) Mental Health facts and statistics [Online] Avaliable at: http://www.mind.og.uk/information-support/types-of-mental-health-problems/statistics-and-facts-about-mental-health/how-common-are-menta-health problems/ [Acsessed:17 march 2017]
Mortimer, A. (2007). Symptom rating scales and outcome in schizophrenia. The British Journal of Psychiatry, [online] 191(50), pp.s7-s14. Available at: http://bjp.rcpsych.org/content/bjprcpsych/191/50/s7.full.pdf [Accessed 19 Mar. 2017].
Muscatello, M., Bruno, A., Pandolfo, G., Micò, U., Scimeca, G., Di Nardo, F., Santoro, V., Spina, E. and Zoccali, R. (2011). Effect of aripiprazole augmentation of clozapine in schizophrenia: A double-blind, placebo-controlled study. [online] Sciencedirect.com. Available at: http://www.sciencedirect.com/science/article/pii/S0920996410016853 [Accessed 20 Mar. 2017].
Nice.org.uk. (2014). Psychosis and schizophrenia in adults: prevention and management | 1-Recommendations | Guidance and guidelines | NICE. [online] Available at: https://www.nice.org.uk/guidance/CG178/chapter/1-Recommendations [Accessed 14 Mar. 2017].
Nice.org.uk. (2014). Psychosis and schizophrenia in adults: prevention and management | Guidance and guidelines | NICE. [online] Available at: https://www.nice.org.uk/guidance/cg178/chapter/1-Recommendations#promoting-recovery-and-possible-future-care-2 [Accessed 20 Apr. 2017].
Sainani, K. (2010). Making Sense of Intention-to-Treat. PM&R, [online] 2(3), pp.209-213. Available at: http://www.pmrjournal.org/article/S1934-1482(10)00006-7/pdf [Accessed 15 Apr. 2017].
Scala, E., Price, C. and Day, J. (2016). An Integrative Review of Engaging Clinical Nurses in Nursing Research. Journal of Nursing Scholarship, [online] 48(4), pp.423-430. Available at: http://onlinelibrary.wiley.com/doi/10.1111/jnu.12223/full [Accessed 13 Mar. 2017].
Shrier, I., Steele, R., Verhagen, E., Herbert, R., Riddell, C. and Kaufman, J. (2014). Beyond intention to treat: What is the right question? Clinical Trials, [online] 11(1), pp.28-37. Available at: http://journals.sagepub.com/doi/pdf/10.1177/1740774513504151 [Accessed 11 Apr. 2017].
Shuttleworth, M. (2009). Longitudinal Study – Studying Long Term Effects. [online] Explorable.com. Available at: https://explorable.com/longitudinal-study [Accessed 10 Apr. 2017].
Socialresearchmethods.net. (2006). Internal Validity. [online] Available at: http://www.socialresearchmethods.net/kb/intval.php [Accessed 16 Mar. 2017]
Sommer, I., Begemann, M., Temmerman, A. and Leucht, S. (2011). Pharmacological Augmentation Strategies for Schizophrenia Patients With Insufficient Response to Clozapine: A Quantitative Literature Review. Schizophrenia Bulletin, [online] 38(5), pp.1003-1011. Available at: https://academic.oup.com/schizophreniabulletin/article/38/5/1003/1897952/Pharmacological-Augmentation-Strategies-for [Accessed 19 Mar. 2017].
Taylor, D., Smith, L., Gee, S. and Nielsen, J. (2011). Augmentation of clozapine with a second antipsychotic – a meta-analysis. Acta Psychiatrica Scandinavica, [online] 125(1), pp.15-24. Available at: http://onlinelibrary.wiley.com/doi/10.1111/j.1600-0447.2011.01792.x/pdf [Accessed 19 Mar. 2017].
Williamson, G. and Whittaker, A. (2014.). Succeeding in literature reviews and research project plans for nursing students. 2nd ed. London: SAGE publications, p.133.



 PRISMA 2009 Flow Diagram
PRISMA 2009 Flow Diagram
Records after duplicates removed
(n = )
Records screened
(n = )
Records excluded
(n = )
Eligibility
Studies included in quantitative synthesis (meta-analysis)
(n = )
Records identified through database searching
(n = )
Additional records identified through other sources
(n = )
Identification
Screening
Full-text articles excluded, with reasons
(n = )
Full-text articles assessed for eligibility
(n = )
Studies included in qualitative synthesis
(n = )
Included
Appendix 2: Paper Information Table
| Title & Authors | Aims | Data collection & Analysis collection | Findings | Commentary |
| Galling, B., Roldán, A., Hagi, K., Rietschel, L., Walyzada, F., Zheng, W., Cao, X., Xiang, Y., Zink, M., Kane, J., Nielsen, J., Leucht, S. and Correll, C. (2017). Antipsychotic augmentation vs. monotherapy in schizophrenia: systematic review, meta-analysis and meta-regression analysis | ||||
| Lewis, S., Barnes, T., Davies, L., Murray, R., Dunn, G., Hayhurst, K., Markwick, A., Lloyd, H. and Jones, P. (2005). Randomized Controlled Trial of Effect of Prescription of Clozapine Versus Other Second-Generation Antipsychotic Drugs in Resistant Schizophrenia. | ||||
| Cipriani, A., Boso, M. and Barbui, C. (2009). Clozapine combined with different antipsychotic drugs for treatment resistant schizophrenia. Cochrane Database of Systematic Reviews. | ||||
| Muscatello, M., Bruno, A., Pandolfo, G., Micò, U., Scimeca, G., Di Nardo, F., Santoro, V., Spina, E. and Zoccali, R. (2011). Effect of aripiprazole augmentation of clozapine in schizophrenia: A double-blind, placebo-controlled study.
Freudenreich, O., Henderson, D., Walsh, J., Culhane, M. and Goff, D. (2007). Risperidone augmentation for schizophrenia partially responsive to clozapine: A double-blind, placebo-controlled trial. |
Ghannt chart
| Sept
16 |
Oct
16 |
Nov
16 |
Dec
16 |
Jan
17 |
Feb
17 |
Mar
17 |
April
17 |
May
17 |
|
| Gain ethics approval | |||||||||
| Nurse participant recruitment | |||||||||
| Patient participant recruitment | |||||||||
| Apply SSCRS intentional act | |||||||||
| Begin patient participant interviews | |||||||||
| Begin nurse participant interviews | |||||||||
| Analyse data | |||||||||
| Participant member checking | |||||||||
| Finalise findings | |||||||||
| Participant de-brief session | |||||||||
| Disseminate findings |
Appenidix 1
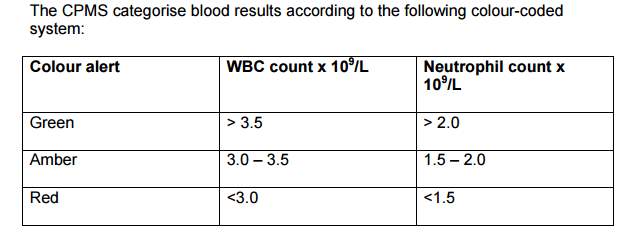
It is important to obtain a green light in patients that are titrating on Clozapine. A red colour alert indicates that a patient needs to stop treatment, they must then have a full blood count taken with white blood cell counts being performed daily, while the patient remains in the red colour group. The patient will need close monitoring for any signs of infection being present during this time.
A patient’s white blood cell count must be less than 3.0 x 109 /L or the neutrophil count is less than 1.5 x 109 /L, this is known as a red alert. A patient who is taking Clozapine medication will need to be discounted immediately.
 (Bleakly and Henry, 2016 pg. 23).
(Bleakly and Henry, 2016 pg. 23).
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allRelated Content
All TagsContent relating to: "Psychology"
Psychology is the study of human behaviour and the mind, taking into account external factors, experiences, social influences and other factors. Psychologists set out to understand the mind of humans, exploring how different factors can contribute to behaviour, thoughts, and feelings.
Related Articles
DMCA / Removal Request
If you are the original writer of this dissertation and no longer wish to have your work published on the UKDiss.com website then please:





