Calcium Phosphate Coated Implants and Osseointegration: A Review
Info: 7336 words (29 pages) Dissertation
Published: 16th Dec 2019
Tagged: Medical Technology
Background
Titanium dental implants have had a high success rate due to good mechanical properties and bio-inertness; however, there are challenging bone conditions when a modified surface may be desirable. Calcium phosphate ceramic coatings have demonstrated potential to compensate for challenging bone conditions such as delayed or impaired bone healing and low bone quantity or density. The increasing universal prevalence of subjects with such challenging bone conditions has enhanced the global use of calcium phosphate coated dental implants. However, the long-term clinical survival of calcium phosphate coated dental implants is questioned because of coating delamination. The purpose of this article is to review the literature on calcium phosphate coated dental implants and its effect on osseointegration. It shall provide a basis for further research on the topic.
Methods
The literature was extensively searched electronically and manually through the electronic databases of the National Library of Medicine (http://www.ncbi.nlm.nih.gov) viz. Medline PubMed and Google Scholar databases to identify articles studying calcium phosphate coated dental implant and calcium phosphate coating techniques. The database was searched for entries from January 2006 to January 2017. In-vitro studies that evaluated the physical, chemical and mechanical properties and in-vivo studies that evaluated the effects of calcium phosphate coatings on titanium dental implants inserted into the bone of animals or humans were included. Randomized controlled clinical trials on humans presenting survival data on the topic of calcium phosphate coated dental implants were also included. Additionally, the reference lists of selected articles and publications in this review were systematically screened.
Results
The electronic search in the Pubmed and Google Scholar database resulted in the identification of 267 titles. The titles were screened for duplication and eliminated. These titles were initially screened for possible inclusion, resulting in 40 publications suitable for further consideration. Screening the abstracts led to 29 full-text articles. Finally, these publications were selected for evaluation. The studies showed that calcium phosphate coating is osteoconductive and can enhance BIC and peri-implant bone formation. Studies showed that plasma sprayed coating are popular and osteoblasts prefer nanocoating’s for adhesion. The studies also demonstrated that calcium phosphate coated dental implants allow early loading and have survival rates comparable to non-coated implants.
Conclusions
Calcium Phosphate has been the most extensively studied coating material because of its biocompatibility and chemical resemblance to human bone. The calcium phosphate coated implants demonstrate enhanced osseointegration during early phases of healing, rapid healing response and ability to overcome challenging conditions like low bone density, irradiation etc. Animal studies show that it is clinically successful compared to noncoated implants. But published long-term survival studies in humans are very limited.
Practical Implications
This review helps practitioners know that calcium phosphate coated implants might be a promising treatment option in compromised cases. But, the clinician should remember that animal study results always may not apply to human bone. Hence, further research should be done on the long-term survival rate of this implant system.
Keywords:
Dental Implants, Osseointegration, Calcium Phosphate, Biomimetic, Coating Techniques, Review, Clinical Trials.
1. INTRODUCTION
Osseointegrated dental implants have been used for the restoration of lost teeth as well as for the rehabilitation of maxillofacial defects in recent decades and also as an anchorage for orthodontic tooth movement with direct bone contact.1 The concept of osseointegration was originally introduced by Brånemark et al.2 in 1969. Albrektsson et al.3 suggested that this was “a direct functional and structural connection between living bone and the surface of a load-carrying implant.” Another clinical definition provided by Zarb and Albrektsson4 proposed that osseointegration was “a process whereby clinically asymptomatic rigid fixation of alloplastic materials is achieved and maintained in bone during functional loading.” Osseointegration consists of a series of bone modeling and remodeling processes. Pure titanium and titanium alloys have been standard materials and most widely used for dental implants because its minimal toxicity, resistance to corrosion, high mechanical resistance, chemical stability, and biocompatibility.5 Integration of titanium implants with the surrounding bone is critical for successful bone regeneration and healing of dental implant. The first generation of successfully used clinical titanium implants, which were machined with a smooth surface texture, now approach 50 years in clinical use.6 It is now well recognized that implants require appropriate surface chemistry and surface topography for enhancing cell attachment, cell growth and tissue formation to enhance the osseointegration process of dental implants for their immediate loading and long-term success.7
The main factors in the clinical success of any biomaterial are its biocompatibility and biofunctionality. The chemical structure and nanocrystallinity of replacement materials determine the success of tissue-implant interactions and long-term reliability. It is well-known that bone consists of Nano sized platelets of crystals of Hydroxyapatite grown in intimate contact with an organic matrix rich in collagen fibers. Fixation of implants to bone tissue using nanocoating’s and nanocomposite coatings with structure, composition, physicochemical, biomechanical, and biological features that mimic those of natural bone is a sound approach for rapid healing and longevity.
Calcium phosphate materials have been researched a lot in recent years because they are chemically identical to bones and teeth. This type of coating material was introduced to combine the high metal strength with the good bioactivity of the calcium phosphate (Ca3(PO4)2) compound.8, 9 They are preferred biomedical materials owing to their excellent biocompatibility, the nontoxicity of their chemical components and their ability to promote osteoconduction and osseointegration.10 The advantage of using calcium phosphate rests in the supply of calcium and phosphate ions which may stimulate the growth of bone tissue on and toward the scaffold. The development of clinically adequate good implant-bone interfacial strength is understood to be a result of this biological interaction of released calcium and phosphate ions.
Calcium phosphates belong to the group of bioactive synthetic materials and its most frequently used are the hydroxyapatite and the tricalcium phosphate due to their crystallographic structures, and chemical composition like the skeletal tissue. Calcium phosphate materials are classified by “resorbability,” that is extent of degradation in vivo. Hydroxyapatite is “non-resorbable” while tricalcium phosphate is “resorbable”.11 A good balance must be reached between the rate of bone growth and solubility of the graft. This would permit adequate mechanical bonding and properties at the implant-tissue interface for long-term survival of an implant or bone graft.12 Hench (1991) stated that the ideal environment for bone growth is established where metal ion release is reduced, good mechanical inter-locking is established, and a bioactive surface is available.11
As the calcium phosphate contacts body fluid, its surface ions can be exchanged with those of the aqueous solution; alternatively, various ions and molecules, such as collagen and proteins, can be adsorbed onto the surface.13 The primary purpose of using calcium phosphate as a bioactive coating is to establish rapid and strong biological attachment to bone. The definition of biological fixation is the process in which the implant or prosthetic components bond firmly to the host bone through bone in-growth and without the use of mechanical fixation or adhesive. Along with compressive forces, to some degree tensile and shear forces are also transmitted through the interface that is through the “bony ingrowth”, improving mechanical properties.
Synthetic calcium phosphate is the obvious choice as an ideal material to replace bone, since it has the same composition and structure as the biogenic apatite, a bone mineral.12 Even though HA coatings have been studied extensively and indicated as one of the ideal implant coatings, it possesses low mechanical strength and fracture toughness, which is an obstacle to its applications in load-bearing areas, hence their long-term prognosis is still controversial.8
There is also an increasing need to minimize the time required for prosthetic rehabilitation in order to reduce patient inconvenience and to accelerate the surrounding bone regeneration process in order to sustain the long-term fixation of implants.14 Dental implants have been widely used in the clinic in recent decades, but there remains a great challenge regarding the relatively low success rates for patients with poor quantity and quality of alveolar bone and with some diseases such as osteoporosis. Atrophic maxilla and mandible bone are less tolerant to the placement of dental implants because of their reduced height and width, hence the presence of sufficient bone volume is an important prerequisite for dental implant placement.15 Currently, concerted efforts are concentrated on accelerating and augmenting bone formation around dental and orthopedic implants through the implantation of various bone grafts/substitutes and/or by modifying the implant surface with osteoinductive coatings, with a view to improving and expediting the establishment of mechanical stability.16, 17
1.1 Bone Implant Interface
Bone is a natural and highly structured organic-inorganic composite material made of collagen fibrils with interspersed hydroxyapatite (HA) nanocrystals for mechanical reinforcement. The mechanical properties of bone tissue are maintained through a continuous remodeling process of bone formation and resorption (bone turnover) that is regulated by “Wolff’s Law”: “Bone is deposited and reinforced at areas of greatest stress”.18 The cells which are responsible for tissue remodeling are osteoblasts (bone-forming) and osteoclasts (bone-resorbing).
Load distribution at the interface between a load-bearing bone implant and natural tissue is affected by the differences in elastic modulus and mechanical strength. A mismatch in stiffness between implants and bone tissue known as stress shielding,19 can have severe consequences that compromise the success of bone implants. A material that can achieve a strong fixation between bone tissue and the implant surface can transfer the load and the stress from the implant to the surrounding bone tissue, thereby ensuring sufficient bone density and strength.20
Bio-inertness was considered as a beneficial property for load-bearing implant surfaces, but the advent of regenerative medicine resulted in increase in the importance of surface modifications. Over the last few decades, various surface modification techniques have been introduced, physical including blasting, etching, oxidizing, titanium (Ti) plasma spraying, and chemical modifications like incorporation of HA or other forms of CaP.21 The quality of the bone implant interface is determined by the quantity of the implant surface in intimate contact with the mineralized bone tissue as well as the mechanical quality of the bone tissue around the interface. Two interfaces contribute to mechanical implant fixation: the implant-coating interface and the coating-bone interface. The implant-coating interface is affected by the mechanical properties of the coating and the bonding strength to the metal substrate are important. The bond strength of the implant-coating interface could be reduced due to the disintegration of the coating.22 Recrystallization of the amorphous phase in calcium phosphate coatings also might result in stress accumulation leading to reduced strength.23 The rate of resorption of the coating also influences the bond strength between bone and implant.24
A systematic review concluded that there was a positive correlation between surface roughness and bone-to-implant contact. The rough topography generally increases the surface area of the implant adjacent to the bone and improves the cell adhesion to the surface, enhancing the bone-to-implant contact and biomechanical integrity. The coated surface of the titanium implant plays a crucial role in determining the biological response of the bone.5 HA-coated implants showed faster healing and bone attachment compared to noncoated implants. Calcium phosphate coated implants also showed excellent clinical outcome when implanted in fresh extraction sites, grafted maxillary sinuses, and areas with poor bone quality.24 It is well established that the calcium phosphate based coating of titanium favors the bone response compared with the uncoated titanium. The calcium phosphate based surfaces bind more attachment proteins, such as fibronectin and vitronectin, for the integrin-mediated binding action of osteoprogenitors compared with titanium surfaces.24
The biological interface reactions can be summarized as follows (Fig. 1).24
Dissolution of calcium phosphate coatings
Reprecipitation of apatite
Ion exchange accompanied by absorption and incorporation of biological molecules
Cell attachment, proliferation, and differentiation
Extracellular matrix formation and mineralization.
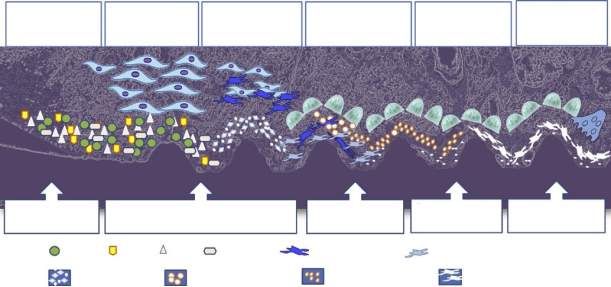
Illustration showing the cellular phenomena at the implant bone interface during the healing of the implant.24
The dissolution of HA coating is a key step to induce the precipitation of bone-like apatite on the implant surface.
1.2 Calcium Phosphate Coating and Peri-implant Wound Healing
There are three major stages involved in direct healing: woven bone formation, adaptation of bone mass to load, and adaptation of bone structure or bone remodeling. The two key processes of the formation of the new bone are Osteoconductivity and osteoinductivity, involving osteoblasts to lay down bone matrix and osteoclasts to remodel the bone tissue. Calcium phosphate coatings act as osteogenic factors and enhance bone integration of metal implants. New bone formation around calcium phosphate coated implants is based on dissolution and local degradation of the calcium phosphate surface soon after implantation followed by secondary crystal growth between the artificial hydroxyapatite and the bone. Early formation of an afibrillar globular calcified layer on the implant surface by osteoblasts which fuses with lamina limitans in which collagen fibers are incorporated is crucial for bonding of the bone to the implant surface. Physicochemical bonding may occur due to reprecipitation of calcium phosphate. (Fig. 2).24
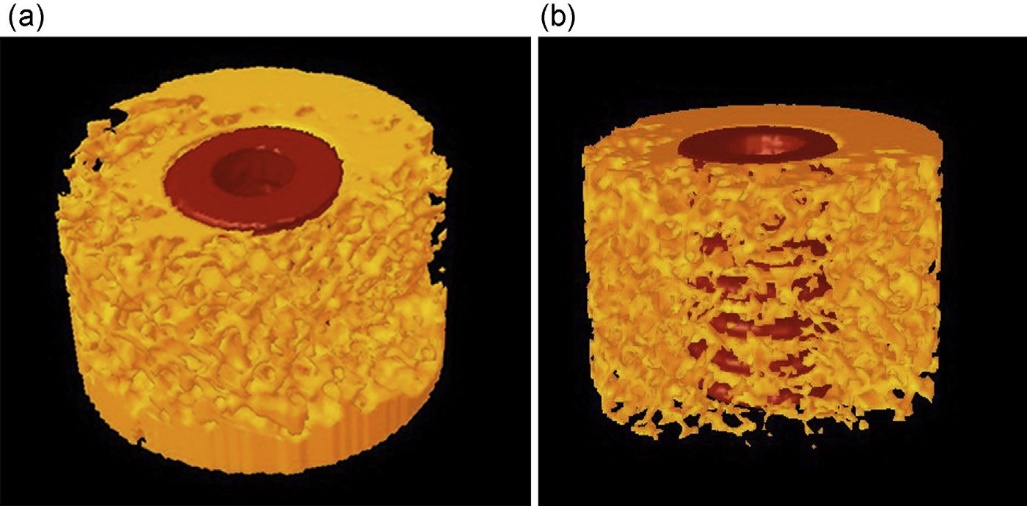
Fig 2. Microcomputed tomography (CT) images showing the bone implant contact around HA-coated (a) and noncoated titanium implants (b) installed (8 weeks healing) in the tibia of beagle dog. Three-dimensional images were generated from micro-CT data for both titanium implants and HA-coated implants.
Enhanced bone formation and accelerated bonding between implant and bone are the advantages for this coating which might be due selective adsorption of serum protein to the surface, which might be responsible for enhanced osteoblast adhesion (Fig. 3).24
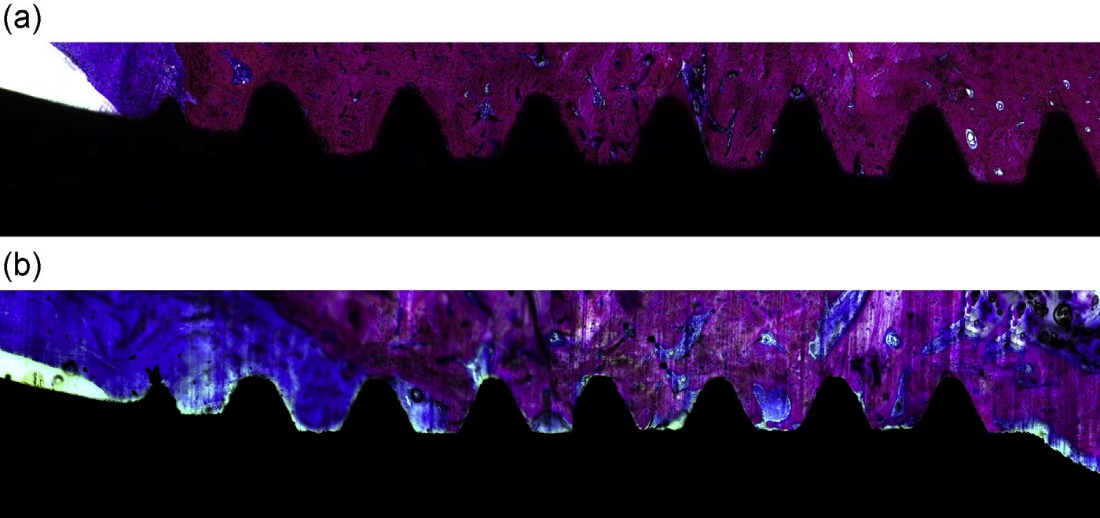
Figure 4.4 Histological section of the HA-coated titanium implant (a) and noncoated titanium implant (b) installed in the mandible of dog. Note the dense bone HA coated around the implant (hematoxylin and eosin and basic fuchsin stained, magnification objective 10).
1.3 Methods of Calcium Phosphate Coating 24
The addition of calcium- and phosphorous-based materials as coatings has received significant attention because these elements are the same as the basic components of the natural bone and coatings can be applied along the implant surfaces by various industrial processing methods. Calcium phosphate coating may undergo extensive dissolution in tissue fluids and demonstrate rapid breakdown around the implant surface. Various coating methods have been tried to achieve optimal quality of the bone implant interface.Several techniques have been used to create the HA coating on metallic implants, such as plasma spraying process, thermal spraying, sputter coating, pulsed laser ablation, dynamic mixing, dip coating, solgel, EPD, biomimetic coating, ion-beamassisted deposition (IBAD), and hot isostatic pressing.

Fig 4. Titanium implant without any surface modification (a). An anodized titanium implant (b) and a Calcium phosphate coated titanium implant (c).
- Plasma sprayed coatings
Plasma-sprayed HA coatings were introduced in the 1980s and are the most frequently used method for clinical application of calcium phosphate coatings. The implant surface is roughened by grit-blasting, shot peening, or etching before plasma spraying. Even though these methods produce coatings with good adhesion strength and fewer pores, they might overheat the metal substrate, thereby changing its mechanical properties.
- Thermal spray coating technique
Thermal spraying of calcium phosphate on the implant devices can be compared with plasma spray-coating technique, having the advantage of high deposition rate and low cost . However, films deposited by thermal spraying have poor coating adherence and nonuniform crystallinity, causing reduced the lifetime of implants.
- Sol Gel Technique
The solgel method represents a simple and low-cost procedure to deposit thin coatings, with homogenous chemical composition onto substrates with large dimensions and complex design. However, the behavior of solgel modifications of loaded osseointegrated implants in the long term remains unknown.
- Sputter deposition
This technique involves the vaporization of atoms or molecules from a solid surface by momentum transfer from bombarding energetic atomic-sized particles. These particles are ions of a gaseous material accelerated in an electric field. Physical sputtering can be divided into several methods, including radiofrequency (RF) magnetron sputtering and high-energy ionic scattering. A common drawback inherent in all these methods is that the deposition rate is very low and the process itself is very slow.
Magnetron sputtering: Magnetron sputtering is a viable thin-film technique as it allows the mechanical properties of titanium to be preserved while maintaining the bioactivity of the coated HA.
RF sputtering: RF magnetron sputtering is largely used to deposit thin films of CaP coatings on titanium implants. RF magnetron sputtering is a very suitable technique to deposit standardized calcium phosphate coatings on titanium substrates. The advantage of this technique is that the coating shows strong adhesion and more retention on titanium.
- Pulsed laser deposition
PLD technique has evolved as an alternative and involves three main steps: ablation of the target material, formation of a highly energetic plume, and the growth of the film on the substrate. The process ensures the titanium surface with increased hardness, corrosion resistance, and a high degree of purity with a standard roughness and thicker oxide layer.
vi. Dip-coating technique
HA can be homogenously coated onto metal substrates to obtain coating thickness in the range of 0.05-0.5 mm. The technique allows uniform coating of HA on the metal surface in short and can be used for substrate with complex shapes. A highly porous surface with bonding strengths of more than 30 MPa can be obtained with this technique.
vii. Ion beam assisted deposition
IBAD method has reduced the dissolution rate of the calcium phosphate coating remarkably, whereas the bonding strength between the layer and Ti substrate has increased. An atomic intermixing layer is formed between the HA coating and Ti substrate during the IBAD method and this chemical bonding may enhance the interfacial adhesive bonding strength.
- Electrophoretic deposition
EPD is a process in which particles in a suspension are coated onto an electrode under the effect of an electric field. A uniform thin coating of HA on titanium with good mechanical strength can be obtained with EPD hydroxyapatite. One of the drawback is the development of porosities, which may later on lead to corrosion and delamination of the titanium caused by penetration of body fluids into the substrate. Even though post-treatment high temperature sintering can be utilized to minimize the porosity by increasing the coating density, chances of formation of cracks in the coating can occur due to the difference in the thermal expansion coefficients.
- Hot isostatic pressing technique
Hot isostatic pressing (HIP) is a method of producing a HA coating on a Ti substrate using pressure to exert the required load at the desired temperature. HIP technique is useful in reducing the porosity and improving the physical and mechanical properties of ceramic coatings.
- Biomimetic precipitation
Biomimetic HA deposition is mimicking the natural process of remineralization of HA, but without involving the cellular and organic levels. Because the biomimetic HA coatings have a low degree of crystallinity and porous structure, their solubility is higher than the dense hydroxyapatite coatings deposited with other methods.
A search of online studies was conducted using PubMed, Medline and Google Scholar databases. A systematic search of the English-language dental literature was performed for articles published between January 2000 to January 2017. The aim was to gather articles of in vitro, in vivo animal studies and human clinical trials pertaining to calcium phosphate coated dental implants. An electronic search was conducted by applying the following free text and Medical Subject Headings (MeSH) Search Methods for Identification of Studies Electronic. The keywords used were “biologically active dental implant surface”, “bioactive dental implant surface”, “dental implant surface modification”, “calcium phosphate coating”, “coating methods”, “Dental Implants”, “Osseointegration”. The search was conducted to identify studies related to firstly, chemical and Phase Composition of Calcium Phosphate, the response to calcium phosphate coating in terms of the bone-implant contact (BIC), osteoblast response, changes occurring on the titanium implant surface and survival rate of coated implants in humans
Criteria for Considering Studies for This Review
Inclusion criteria
- Current developments published during January 2000 to January 2017.
- Physicochemical studies of calcium phosphate dental implant surfaces.
- Titanium implant surfaces coated with calcium phosphate.
- In vivo study, in vitro illustrating cellular responses in different implant surfaces such as smooth or rough surfaces, evaluation of the effect of the coatings on bone formation or osseointegration.
- Studies related to osseointegration and clinical performance from different implant surface modification techniques.
- Studies of which complete text could be assessed
- Published in the English language.
Exclusion criteria
- Use of calcium phosphate as graft to fill the defect before or after implant placement
- Intentional creation of peri-implant defects
- Evaluation of the effect of biomolecular coatings on soft tissue, regeneration, ridge augmentation or sinus floor elevation
- In vivo studies including sample size less than 5 were excluded
- In vitro studies include agents that do not use bone-related cells
- Studies whose title did not meet aim of present review
After applying search strategy, a total of 267 studies displaying the used terms were found. All studies were assigned to full-text analysis. The extracted data were assigned for comparison. By applying inclusion and exclusion criteria total 29 studies were selected. Selection of relevant studies was conducted as follows: Initial assessment of each publication for relevance using the information presented in the abstract. When the abstract passed the inclusion criteria, a print of full paper was obtained. Data extraction was done by one reviewer. After checking studies that did not fulfill selection criteria, the final outcome of the search was combined.
3. RESULTS
The electronic search in the Pubmed and Google Scholar database resulted in the identification of 267 titles. The titles were screened for duplication and then inclusion, resulting in 40 publications suitable for further consideration. Screening the abstracts led to 29 full-text articles and were evaluated. The in vitro studies show that calcium phosphate is osteoconducive and the surface morphology affects osseointegration. Further animal studies showed that calcium phosphate coating confirms the in vitro findings and show that it can enhance BIC and peri-implant bone formation. The studies also demonstrated that calcium phosphate coated dental implants allow early loading, preserve crestal bone better preventing pocket formation leading to better long-term survival rates.
3.1 In Vitro and In Vivo Studies
Okamoto et al. reported that a cells have higher affinity and adhere more to hydroxyapatite than to uncoated titanium.25 Rouahi et al. studied the growth of Saos-2 cells on discs of microporous and nonporous hydroxyapatite in comparison to titanium and found that the surface morphology affects the behavior of the cells.26 Yang et al. reported that porous surfaces had greater cell proliferation and type I collagen synthesis than on dense ones. This can be explained as there increased surface area available for greater protein absorption and for cell attachment.27 Richard et al. cultured cells on hydroxyapatite thin films produced using electrodeposition and studied cell morphology, cell viability, cell proliferation over 28 days. The calcium phosphate coating compared to the titanium plate had enhanced differentiation of osteoblast cells.28 Wang et al. studied the effect of the phase composition of calcium phosphate ceramics on osteoblast behavior. The compositions studied were pure hydroxyapatite, a 70/30 mixture of hydroxyapatite and tricalcium phosphate, and a 35/65 mixture of hydroxyapatite and tricalcium phosphate and pure tricalcium phosphate. In their study, the phase composition of the ceramics did not have a significant effect on the expression of the osteonectin and production of bone sialoprotein and osteocalcin in SaOS-2 cells.29
The first and essential step in vivo tests for bone tissue-implant interface studies is using osteoblast cells as they play an important in the osteointegration of the implant. They produce extracellular matrix and to control its mineralization, regulating the “ingrowth” of bone to the implant. In the trabecular bone of mature miniature pigs, Wong et al. compared the osseointegration of commercial implants for 12 weeks and showed that the hydroxyapatite coated implant demonstrate excellent osseointegration.30 Similarly successful osseointegration of hydroxyapatite coated implant was placed within living bone was shown by Cao et al.31
In sheep pelvis, Langhoff et al. compared osseointegration of 6 modified implant surfaces for 8 weeks. A clear tendency of calcium phosphate coated implants was seen to show better BIC values at 8 weeks compared to titanium or zirconia.10 Alghamdi et al demonstrated in the mandibles of dogs that Nano calcium phosphate coated implants showed significantly higher bone volume in the inner zone than noncoated implants.10 Lee et al. studied in rabbit tibiae the effect of calcium phosphate and type I collagen coating on peri-implant bone formation. After 6 weeks of implant placement calcium phosphate coating surfaces showed greater peri-implant bone formation and BIC. 32
Other histometric studies in animal models comparing hydroxyapatite-coated implants to titanium implants have shown that bone adapts in much less time and the mineralizes directly on calcium phosphate surface without fibrous tissue layer formation.33 Additionally, in an animal study increased coronal bone growth was observed with hydroxyapatite-coated implants than titanium implants. To prevent peri-implant saucerization and subsequent pocket formation, it is clinically essential to maintain a bony osseous crest.34
3.2 Calcium Phosphate Coating and Challenging Bone Conditions
- Osteoporosis
Many systemic conditions like osteoporosis affect the osseointegration of dental implants. Alghamdi et al evaluated the effect of a calcium phosphate coating on osseointegration in healthy and osteoporotic rats. Implants were placed in femoral condyles and after 8 weeks’ bone volume and histomorphometric bone area were lower around non-coated implants in osteoporotic rats compared with healthy rats. Push-out tests also revealed significantly enhanced implant fixation for calcium phosphate coated compared with non-coated implants in both osteoporotic (i.e., 2.9-fold) and healthy rats (i.e., 1.5-fold), with no difference between osteoporotic and healthy rats for calcium phosphate coated implants. Calcium Phosphate coating increased bone-to-implant contact compared with that in noncoated implants in both osteoporotic (i.e., 1.3-fold) and healthy rats (i.e., 1.4-fold).35 Analysis of the data obtained showed that thin calcium phosphate coatings improve osseointegration in both healthy and osteoporotic conditions.
- Irradiated Bone
Radiotherapy is known to affect the quality of bone and compromise the integration of implant leading to implant loss. Li et. al investigated the osseointegration of calcium phosphate nanocrystals coated implants in irradiated bone. Sixteen rabbits were randomly assigned to receive implants with dual acid-etched surface or dual acid-etched surface discretely deposited of nanoscale calcium-phosphate crystals as control or Nano-calcium phosphate groups. The implants were placed in left leg of all the rabbits one week after receiving 15Gy radiation. Implant stability quotient (ISQ), ratio of bone volume to total volume (BV/TV), bone growth rate, and bone-to-implant contact (BIC) were evaluated at 4 and 12 weeks. The Nano calcium phosphate coated group showed significantly higher ISQ (week 12, = 0.031) and bone growth rate (week 6, = 0.021; week9, = 0.001) than that in control group. There were no significant differences in BV/TV and BIC between the two groups. Titanium implant surface modified with calcium phosphate nanocrystals provides a possible alternative to improve bone healing around implant in irradiated bone.36
3.3 Clinical Trial
Bacterial colonization on surface of dental implants may lead to inflammatory reactions, which cause the loss of osseointegration. Peri-implantitis is defined as ‘‘an inflammatory process affecting the soft and hard tissues surrounding an osseointegrated implant, resulting in the rapid loss of the supporting bone, bleeding, and suppuration.” The implant surface chemical nature and topography plays a role in peri-implant disease development. Rough surfaces on superstructures and abutments are stated to accumulate and retain more bacterial plaque than smooth surfaces and often cause inflammation of surrounding tissues.37 The rough surfaces provide fortes for the bacteria for protection from host defenses and routine oral hygiene treatments. Calcium phosphate coatings increase the surface roughness of implants. When compared with noncoated implants, coated implants have reported to be at a higher risk for failure, due to peri-implant diseases. 38, 39
Morris et al. studied the periodontal response to Calcium phosphate coated and non-coated implants for 36 months.40 Calcium phosphate coated endosseous dental implants has gained in popularity but their use remains highly controversial. The concerns are that the coating may separate from the substructure, undergo dissolution in tissue fluids, is susceptible to bacterial colonization due to their roughness and hydrophilicity and/or lead to rapid osseous breakdown around the implant, peri-implantitis and implant failure. 32 clinical research centers placed more than 2900 implants and were randomized to maxillary anterior, mandibular anterior, and mandibular posterior. There was no clinically significant difference between the coated and non– calcium phosphate coated implants followed for a period from 3 through 36 months. No adverse periodontal responses where seen associated with Calcium phosphate coated implants were seen for 36 months.40
4. CONCLUSION
Calcium Phosphate has been the most researched coating material because of its biocompatibility and chemical resemblance to human bone. Osseointegration and implant stability is affected greatly by implant surface. Altered implant surface through surface treatments is osteoconductive and promote osteogenesis by increasing the surface area, enhancing cellular activity leading to more bone attachment. The calcium phosphate coated implants produce early implant stability due to rapid healing responses, faster bone attachment, leading to a high clinical survival rate when compared to noncoated implants. They also demonstrate ability to offer treatment in compromised cases like atrophic maxilla or mandible, osteoporosis and bone after irradiation. Dissolution in tissue fluids leading to rapid breakdown around the implant surface is one of its major drawback. To overcome these drawbacks, currently research is being carried to alter the composition as well as to develop newer method of calcium phosphate deposition. Available literature supports use of calcium phosphate coated implants with in vitro and animal studies. But published success and long term survival rate of these implants in human beings is not sufficient. Further studies are required to evaluate the long-term survival rates in vivo clinical trials to improve coating properties along with the preclinical research to provide better understanding of the bone responses to the coated implant surfaces.
REFERENCES
1. Branemark PI. Osseointegration and its experimental background. J Prosthet Dent 1983;50(3):399-410.
2. Branemark PI, Adell R, Breine U, et al. Intra-osseous anchorage of dental prostheses. I. Experimental studies. Scand J Plast Reconstr Surg 1969;3(2):81-100.
3. Albrektsson T, Branemark PI, Hansson HA, Lindstrom J. Osseointegrated titanium implants. Requirements for ensuring a long-lasting, direct bone-to-implant anchorage in man. Acta Orthop Scand 1981;52(2):155-70.
4. Zarb G, Albrektsson T. Osseointegration: a requiem for the periodontal ligament. Int J Periodont Rest Dent 1991;11(1):88-91.
5. Xuereb M, Camilleri J, Attard NJ. Systematic Review of Current Dental Implant Coating Materials and Novel Coating Techniques. International Journal of Prosthodontics 2015;28(1):51-59.
6. Ballo AM, Omar O, Xia W, Palmquist A. Dental implant surfaces–physicochemical properties, biological performance, and trends. Implant Dentistry-A Rapidly Evolving Practice: InTech; 2011.
7. Xie C, Lu H, Li W, Chen FM, Zhao YM. The use of calcium phosphate-based biomaterials in implant dentistry. J Mater Sci Mater Med 2012;23(3):853-62.
8. Oshida Y, Tuna EB, Aktoren O, Gencay K. Dental implant systems. Int J Mol Sci 2010;11(4):1580-678.
9. Le Guehennec L, Soueidan A, Layrolle P, Amouriq Y. Surface treatments of titanium dental implants for rapid osseointegration. Dent Mater 2007;23(7):844-54.
10. Al-Sanabani JS, Madfa AA, Al-Sanabani FA. Application of calcium phosphate materials in dentistry. Int J Biomater 2013;2013:876132.
11. Hench LL. Bioceramics: from concept to clinic. Journal of the american ceramic society 1991;74(7):1487-510.
12. Ben-Nissan B, Choi AH. Sol-gel production of bioactive nanocoatings for medical applications. Part 1: an introduction. Nanomedicine (Lond) 2006;1(3):311-9.
13. Choi AH, Ben-Nissan B. Sol-gel production of bioactive nanocoatings for medical applications. Part II: current research and development. Nanomedicine (Lond) 2007;2(1):51-61.
14. Gapski R, Wang HL, Mascarenhas P, Lang NP. Critical review of immediate implant loading. Clin Oral Implants Res 2003;14(5):515-27.
15. Chiapasco M, Casentini P, Zaniboni M. Bone augmentation procedures in implant dentistry. Int J Oral Maxillofac Implants 2009;24 Suppl:237-59.
16. Hallman M, Thor A. Bone substitutes and growth factors as an alternative/complement to autogenous bone for grafting in implant dentistry. Periodontol 2000 2008;47:172-92.
17. Liu Y, de Groot K, Hunziker EB. Osteoinductive implants: the mise-en-scene for drug-bearing biomimetic coatings. Ann Biomed Eng 2004;32(3):398-406.
18. Ahn AC, Grodzinsky AJ. Relevance of collagen piezoelectricity to “Wolff’s Law”: a critical review. Med Eng Phys 2009;31(7):733-41.
19. Ramakrishna S, Mayer J, Wintermantel E, Leong KW. Biomedical applications of polymer-composite materials: a review. Composites science and technology 2001;61(9):1189-224.
20. Bosco R, Van Den Beucken J, Leeuwenburgh S, Jansen J. Surface Engineering for Bone Implants: A Trend from Passive to Active Surfaces. Coatings 2012;2(4):95-119.
21. Wennerberg A, Albrektsson T. Effects of titanium surface topography on bone integration: a systematic review. Clin Oral Implants Res 2009;20 Suppl 4:172-84.
22. Mohseni E, Zalnezhad E, Bushroa AR. Comparative investigation on the adhesion of hydroxyapatite coating on Ti–6Al–4V implant: A review paper. International Journal of Adhesion and Adhesives 2014;48:238-57.
23. Ogiso M, Yamashita Y, Matsumoto T. Microstructural changes in bone of HA-coated implants. J Biomed Mater Res 1998;39(1):23-31.
24. Anil S, Venkatesan J, Shim MS, Chalisserry EP, Kim SK. 4 – Bone response to calcium phosphate coatings for dental implants A2 – Piattelli, Adriano. Bone Response to Dental Implant Materials: Woodhead Publishing; 2017. p. 65-88.
25. Okamoto K, Matsuura T, Hosokawa R, Akagawa Y. RGD peptides regulate the specific adhesion scheme of osteoblasts to hydroxyapatite but not to titanium. J Dent Res 1998;77(3):481-7.
26. Rouahi M, Champion E, Hardouin P, Anselme K. Quantitative kinetic analysis of gene expression during human osteoblastic adhesion on orthopaedic materials. Biomaterials 2006;27(14):2829-44.
27. Yang Y, Tian J, Deng L, Ong JL. Morphological behavior of osteoblast-like cells on surface-modified titanium in vitro. Biomaterials 2002;23(5):1383-9.
28. Richard D, Dumelie N, Benhayoune H, et al. Behavior of human osteoblast-like cells in contact with electrodeposited calcium phosphate coatings. J Biomed Mater Res B Appl Biomater 2006;79(1):108-15.
29. Wang C, Duan Y, Markovic B, et al. Phenotypic expression of bone-related genes in osteoblasts grown on calcium phosphate ceramics with different phase compositions. Biomaterials 2004;25(13):2507-14.
30. Wong M, Eulenberger J, Schenk R, Hunziker E. Effect of surface topology on the osseointegration of implant materials in trabecular bone. J Biomed Mater Res 1995;29(12):1567-75.
31. Cao N, Ma Q-S, Sui J-L, et al. The experiment of plasma-sprayed HA coatings on carbon/carbon composites in bone. Surface Review and Letters 2006;13(04):423-28.
32. Meng HW, Chien EY, Chien HH. Dental implant bioactive surface modifications and their effects on osseointegration: a review. Biomark Res 2016;4:24.
33. Gammage DD, Bowman AE, Meffert RM, Cassingham RJ, Davenport WA. Histologic and scanning electron micrographic comparison of the osseous interface in loaded IMZ and Integral implants. Int J Periodontics Restorative Dent 1990;10(2):124-35.
34. Kohri M, Cooper EP, Ferracane JL, Waite DF. Comparative study of hydroxyapatite and titanium dental implants in dogs. J Oral Maxillofac Surg 1990;48(12):1265-73.
35. Alghamdi HS, Cuijpers VM, Wolke JG, van den Beucken JJ, Jansen JA. Calcium-phosphate-coated oral implants promote osseointegration in osteoporosis. J Dent Res 2013;92(11):982-8.
36. Li JY, Pow EH, Zheng LW, et al. Effects of calcium phosphate nanocrystals on osseointegration of titanium implant in irradiated bone. Biomed Res Int 2015;2015:783894.
37. Norowski PA, Jr., Bumgardner JD. Biomaterial and antibiotic strategies for peri-implantitis: a review. J Biomed Mater Res B Appl Biomater 2009;88(2):530-43.
38. Piattelli A, Cosci F, Scarano A, Trisi P. Localized chronic suppurative bone infection as a sequel of peri-implantitis in a hydroxyapatite-coated dental implant. Biomaterials 1995;16(12):917-20.
39. Madi M, Zakaria O, Noritake K, Fuji M, Kasugai S. Peri-implantitis progression around thin sputtered hydroxyapatite-coated implants: clinical and radiographic evaluation in dogs. Int J Oral Maxillofac Implants 2013;28(3):701-9.
40. Morris HF, Ochi S, Spray JR, Olson JW. Periodontal-type measurements associated with hydroxyapatite-coated and non-HA-coated implants: uncovering to 36 months. Ann Periodontol 2000;5(1):56-67.
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allRelated Content
All TagsContent relating to: "Medical Technology"
Medical Technology is used to enhance the medical care and treatment that patients are given in healthcare settings. Medical Technology can be used to identify, diagnose and treat medical conditions and illnesses.
Related Articles
DMCA / Removal Request
If you are the original writer of this dissertation and no longer wish to have your work published on the UKDiss.com website then please: